Arthroscopy For sports injuries: when Is It required?

A player is holding his knee in pain.
Sports injuries are common. A twisted knee during a football match, a shoulder that gives out during a throw, an ankle rolled on an uneven surface, these things happen to professional athletes and weekend warriors alike. Most of the time, rest, physiotherapy, and medication are enough. The body heals, and you get back to your activity.
But sometimes it doesn't work out that way. The pain lingers. The swelling keeps returning. The joint feels unstable, like it might buckle under you. When conservative treatment fails to resolve a joint injury after 4-6 weeks, or when imaging reveals structural damage inside the joint, we start considering arthroscopy.
I've performed hundreds of arthroscopic procedures over my career at KDSG Superspeciality Hospitals, Noida. It remains one of the most valuable tools in sports medicine, not because it's high-tech (though it is), but because it lets us see exactly what's wrong inside a joint and fix it through incisions smaller than a centimeter. The precision is hard to match with any other approach.
What Is arthroscopy?
Arthroscopy is a minimally invasive surgical technique that allows direct visualization and treatment of problems inside a joint. The word itself comes from Greek — "arthro" (joint) and "skopein" (to look).
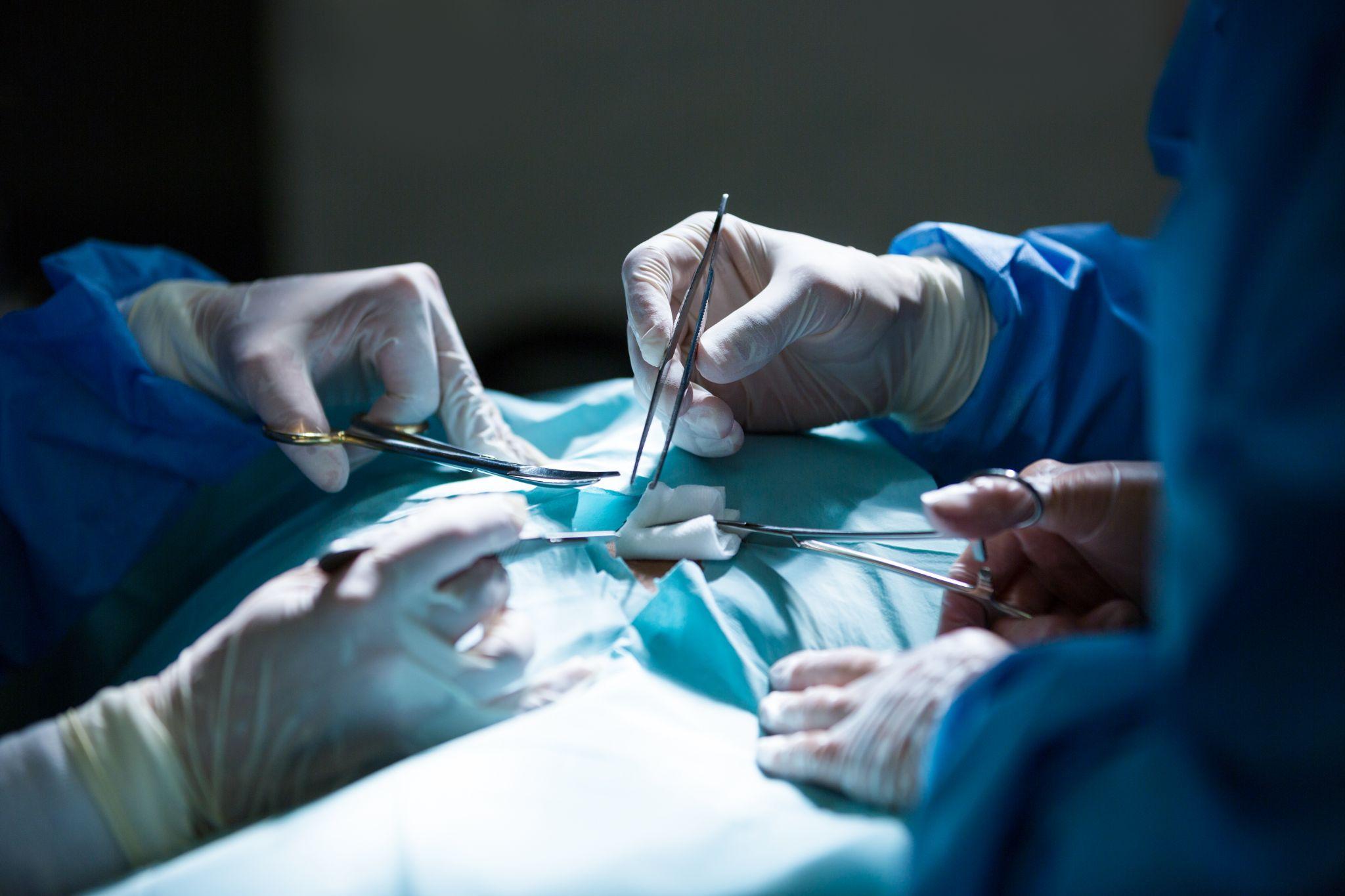
Here's the procedure in practical terms: I make a small incision (usually 5-7 mm) near the joint and insert an arthroscope, a narrow tube with a camera and light source at its tip. This camera transmits high-definition images to a monitor, giving me a magnified, real-time view of the entire interior of the joint: cartilage surfaces, ligaments, menisci, synovial lining, and any abnormal tissue.
If the diagnostic images reveal something that needs repair, I make one or two additional small incisions to insert specialized instruments, tiny shavers, graspers, suture anchors, and radiofrequency probes. The repair happens under direct visualization, meaning I can see exactly what I'm working on at all times.
Arthroscopy is most commonly used for:
- Knee — the most frequent site, accounting for roughly 50% of all arthroscopic procedures
- Shoulder, second most common, particularly for rotator cuff and labral repairs
- Ankle, for cartilage damage, impingement, and loose bodies
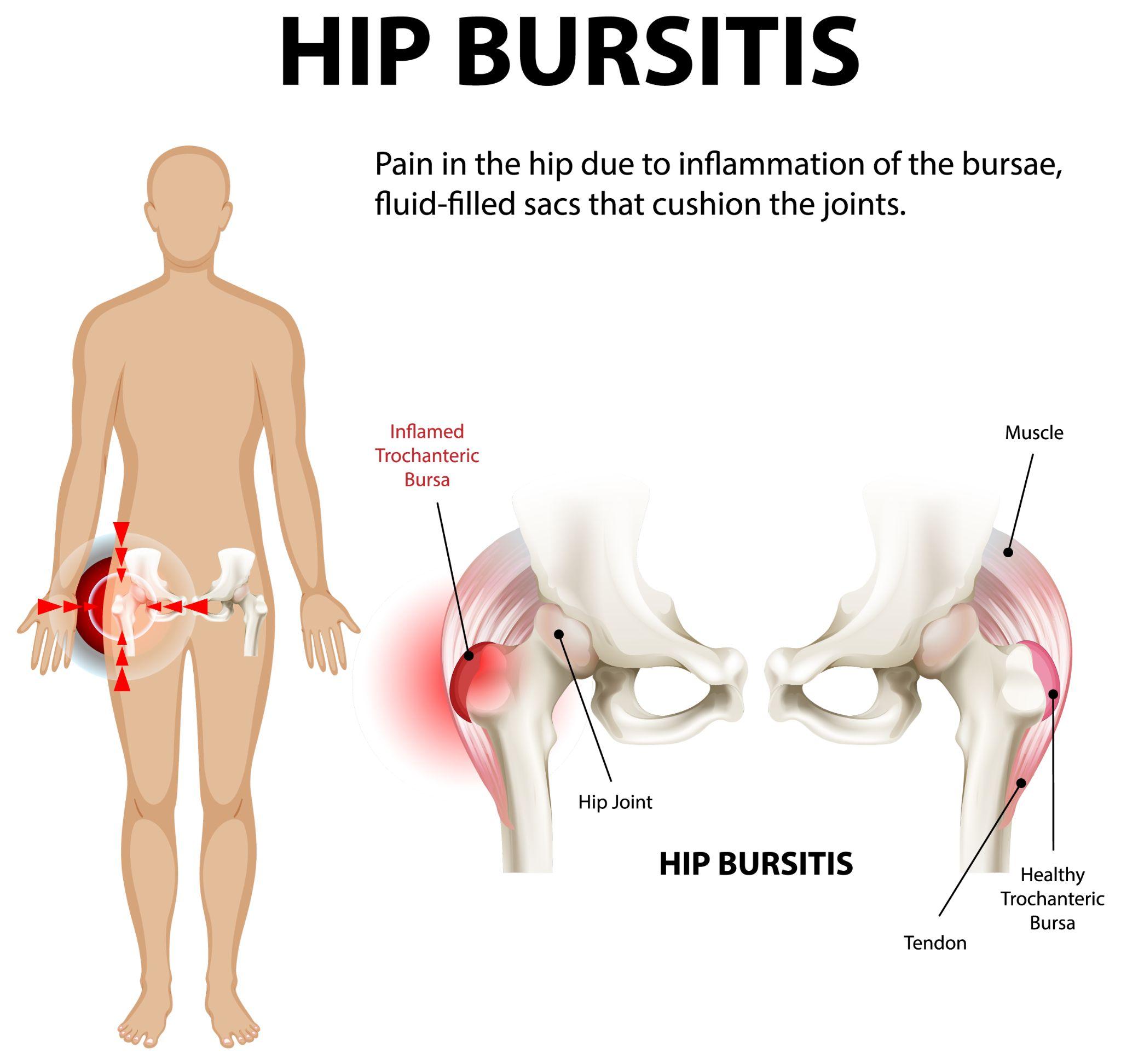
- Hip — increasingly used for labral tears and femoroacetabular impingement
- Wrist and elbow, less common but useful for specific conditions
Because the incisions are small, tissue disruption is minimal. Patients experience less post-operative pain, have smaller scars, and recover faster compared to traditional open surgery. Most procedures take between 30 minutes and 2 hours, depending on the joint involved and the complexity of the problem.
Common sports injuries treated with arthroscopy
Arthroscopy has become the standard approach for diagnosing and treating a wide range of sports-related joint injuries. Here are the conditions I treat most frequently:
1. torn ligaments (ACL, PCL)
Ligament tears are among the most common sports injuries I see, particularly ACL (anterior cruciate ligament) tears in the knee. These typically happen during sudden deceleration, pivoting, or awkward landings, common in football, basketball, kabaddi, and cricket.
During arthroscopic ACL reconstruction, I remove the torn ligament and replace it with a graft — usually harvested from the patient's own hamstring tendon or patellar tendon. The arthroscope allows precise placement of the graft using tunnels drilled through the bone, with accuracy that's difficult to achieve through open surgery.
Recovery from ACL reconstruction typically takes 6-9 months before return to competitive sports, with structured physiotherapy beginning within the first week after surgery.
2. meniscus tears
The meniscus is a crescent-shaped piece of cartilage that acts as a shock absorber between your thigh bone and shin bone. Each knee has two, medial (inner) and lateral (outer). Sports that involve quick direction changes, pivoting, and deep squatting frequently tear the meniscus.
Through arthroscopy, I can either repair the tear (suturing it back together) or trim the damaged portion (partial meniscectomy). The decision depends on the tear's location, pattern, and the patient's age and activity level. Tears in the outer third of the meniscus have a blood supply and heal well with repair. Tears in the inner two-thirds typically require trimming because that zone lacks the blood supply needed for healing.
Recovery after meniscus repair takes 4-6 weeks for basic activities, though return to sports may take 3-4 months. After partial meniscectomy, most patients walk without crutches within a week.
3. shoulder labral tears
The labrum is a ring of fibrocartilage that deepens the shoulder socket, helping keep the ball of the upper arm bone centered. Overhead athletes, cricket bowlers, tennis players, swimmers, volleyball players — are particularly susceptible to labral tears. So are people who dislocate their shoulders.
Arthroscopic labral repair involves reattaching the torn labrum to the socket rim using small suture anchors. The procedure restores shoulder stability and reduces the risk of recurrent dislocations. Without repair, a torn labrum often leads to repeated shoulder instability episodes that progressively stretch the joint capsule.
4. cartilage damage
Articular cartilage, the smooth white tissue covering the bone ends inside a joint, can be damaged by a single traumatic event or by repetitive wear. Athletes often develop focal cartilage defects from impact injuries.
Arthroscopy allows me to assess the extent of cartilage damage directly (MRI sometimes underestimates it) and perform treatments ranging from debridement (smoothing out rough areas) to microfracture (creating tiny holes in the bone to stimulate new cartilage growth) to cartilage transplantation in select cases.
5. loose bodies in the joint
A hard impact, a cartilage fragment that breaks free, or a piece of bone that chips off — any of these can leave a loose body floating inside the joint. These fragments cause intermittent locking, catching, and sharp pain as they wedge between the moving surfaces.
Arthroscopic removal is straightforward. Once I locate the fragment on the camera, I use a grasper to extract it through a small portal. Relief is often immediate, patients frequently notice the locking sensation is gone within days of surgery.
6. synovial problems and joint inflammation
Sometimes the synovial lining of a joint (the tissue that produces joint fluid) becomes inflamed, thickened, or develops abnormal growths. This can happen in conditions like synovial chondromatosis or pigmented villonodular synovitis (PVNS). Arthroscopy allows both biopsy and removal of the abnormal tissue.
When Do You really need arthroscopy?

A woman is holding her shoulder in pain.
I don't recommend arthroscopy as a first option. Conservative treatment, rest, ice, anti-inflammatory medications, physiotherapy — resolves the majority of sports injuries. Arthroscopy enters the picture when conservative measures have been given adequate time and haven't worked, or when the nature of the injury demands surgical intervention from the outset (like a complete ACL tear in a young athlete who wants to return to sport).
Here are the specific situations where I consider arthroscopy:
1. persistent joint pain despite conservative treatment
If you've rested the joint, completed 4-6 weeks of physiotherapy, taken appropriate medications, and the pain hasn't improved, or has worsened, there's likely structural damage that won't heal on its own. Cartilage tears, ligament injuries, and chronic synovial inflammation often fall into this category. Arthroscopy lets me see the source of pain directly and address it.
2. recurrent swelling and inflammation
A joint that swells repeatedly — particularly after activity, is telling you something is wrong internally. The swelling represents an inflammatory response to ongoing damage, whether it's a cartilage flap irritating the synovium, a partially torn ligament that's unstable, or loose fragments inside the joint. If the swelling returns despite rest and anti-inflammatories, arthroscopic evaluation is warranted.
3. joint instability
If your knee feels like it might give out during walking or pivoting, or your shoulder feels like it might slip out of its socket during overhead movements, you likely have ligament or labral damage. This instability doesn't just affect performance, it puts you at risk for secondary injuries. A knee that buckles can tear additional structures; a shoulder that partially dislocates can damage the cartilage and bone.
4. limited range of motion
When you can't fully bend, straighten, or rotate a joint — and physiotherapy hasn't restored the motion, something mechanical is usually blocking it. Scar tissue, a displaced meniscal tear, a loose body, or an inflamed synovial fold can all physically obstruct normal joint movement. Arthroscopy can identify and remove the obstruction.
5. locking or catching sensation
A joint that suddenly locks, refusing to bend or straighten — or catches with a painful click during movement usually has a mechanical problem: a torn meniscus flap, a loose body, or a displaced cartilage fragment. These don't resolve with rest or medication. They need to be addressed surgically, and arthroscopy is the least invasive way to do it.
Risks and complications of arthroscopy
Arthroscopy is one of the safest surgical procedures we perform, but no surgery is without risk. Patients should be aware of:
- Post-operative swelling and stiffness, this is expected and typically resolves within 1-2 weeks with ice, elevation, and gentle range-of-motion exercises.
- Infection, the risk is low (less than 1% in most studies), but any redness, warmth, increasing pain, or drainage from the incision sites should be reported immediately.
- Temporary nerve irritation — numbness or tingling near the incision sites occasionally occurs and almost always resolves within a few weeks.
- Blood clots (deep vein thrombosis), rare with arthroscopy, but the risk increases if the patient is immobile for extended periods after surgery. Early mobilization and sometimes blood thinners are used to prevent this.
- Stiffness from inadequate rehabilitation, this is more of a rehabilitation failure than a surgical complication. Following the prescribed physiotherapy protocol is essential.
Overall, complication rates for arthroscopy are significantly lower than for open joint surgery. The small incisions, minimal tissue disruption, and faster return to activity all contribute to a safer profile.
Benefits of arthroscopy for sports injuries
Why has arthroscopy become the preferred approach in sports medicine? Several reasons:
- Minimal tissue damage. The incisions are 5-7 mm, compared to 10-15 cm for traditional open surgery. Less cutting means less pain, less bleeding, and less scar tissue formation.
- Superior visualization. The arthroscope provides a magnified, well-lit view of the entire joint interior. I often see details arthroscopically that weren't visible even on an MRI — subtle cartilage fibrillation, synovial changes, early ligament fraying.
- Precise repair. Working under direct camera visualization allows exact placement of sutures, anchors, and grafts. This precision translates to better surgical outcomes and more durable repairs.
- Faster recovery. Most patients leave the hospital the same day. Return to desk work typically happens within a week. Return to full sports activity depends on the procedure but is substantially faster than after open surgery.
- Lower complication rates. Less tissue disruption means lower infection risk, less blood loss, and reduced formation of adhesions (scar tissue bands that can restrict joint motion).
Recovery after arthroscopy
Recovery timelines vary depending on the joint treated and the procedure performed. Here's what the typical process looks like:
Days 1-3: Rest, ice, elevation, and pain management. The joint will be swollen and stiff. Most patients use crutches for knee procedures and a sling for shoulder procedures during this initial phase. I prescribe a specific set of gentle range-of-motion exercises to begin immediately, keeping the joint completely immobile is counterproductive.
Weeks 1-3: Physiotherapy begins with a focus on reducing swelling, restoring range of motion, and reactivating the muscles around the joint. For simple procedures like loose body removal, many patients are walking normally by this point.
Weeks 4-8: Strengthening exercises progressively increase. Patients typically return to most daily activities. For meniscus repairs and ligament reconstructions, this phase involves controlled loading under physiotherapy supervision.
Months 3-9 (for ligament reconstructions): Gradual return to sport-specific training. The graft needs time to mature and integrate with bone. Rushing this phase risks re-injury. I use functional testing, single-leg hop tests, strength measurements, agility assessments — to determine when a patient is genuinely ready to return to competitive sport.
Most patients with simpler procedures (debridement, loose body removal, partial meniscectomy) return to their usual routines within 2-4 weeks. ACL reconstruction and complex shoulder repairs require longer timelines and more structured rehabilitation.
When to See an orthopedic specialist

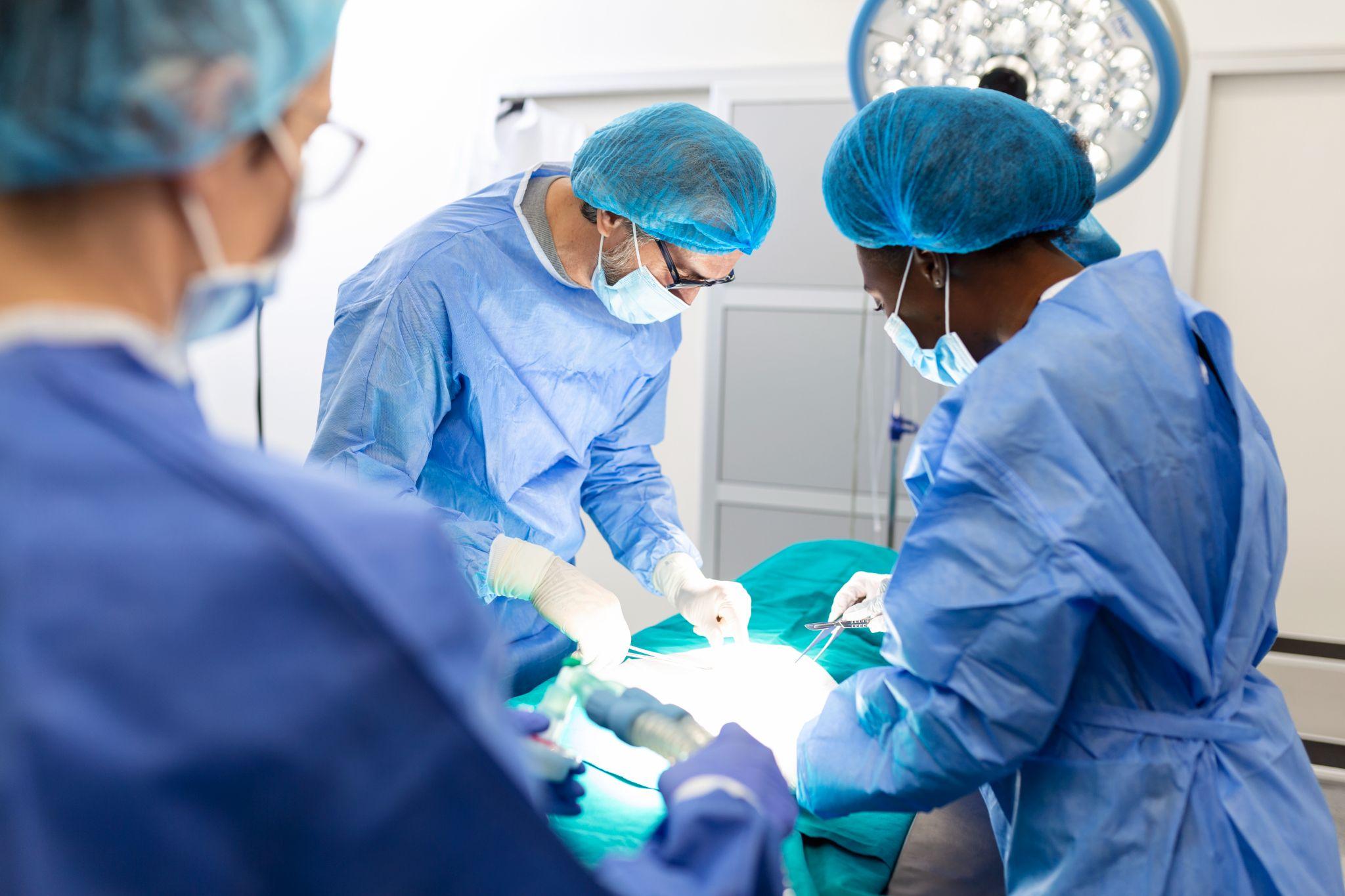
A team of surgeons doing arthroscopy on a patient.
Don't wait until a sports injury becomes a chronic problem. Seeing an orthopedic specialist early allows accurate diagnosis and prevents secondary damage. Get an evaluation if:
- Joint pain persists beyond 2-3 weeks despite rest and home treatment
- The joint swells repeatedly after activity
- You've lost range of motion that hasn't returned with stretching
- The joint feels unstable or like it might buckle
- You experience locking, catching, or a sensation of something "moving around" inside the joint
- You heard or felt a "pop" at the time of injury, followed by rapid swelling
Early assessment, including clinical examination and often an MRI, can distinguish between injuries that will heal with conservative management and those that need surgical intervention. The longer structural damage goes untreated, the more difficult it becomes to achieve a full recovery.
Final thoughts
Sports injuries are an unavoidable part of an active life. Most heal with time, rest, and structured rehabilitation. But when conservative treatment reaches its limits — when the pain persists, the swelling returns, or the joint simply isn't stable, arthroscopy provides a way to diagnose and repair the damage with minimal disruption to your body and your life.
If you're dealing with a joint injury that isn't improving, or if you've been told you might need surgery and want to understand your options, I'm available for consultation at KDSG Superspeciality Hospitals, Noida. The goal is always the same: accurate diagnosis, appropriate treatment, and getting you back to the activities that matter to you, safely and with lasting results.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.