Why Are You having Hip pain? common causes in adults explained

Elderly woman sitting and holding her lower back and hip in pain
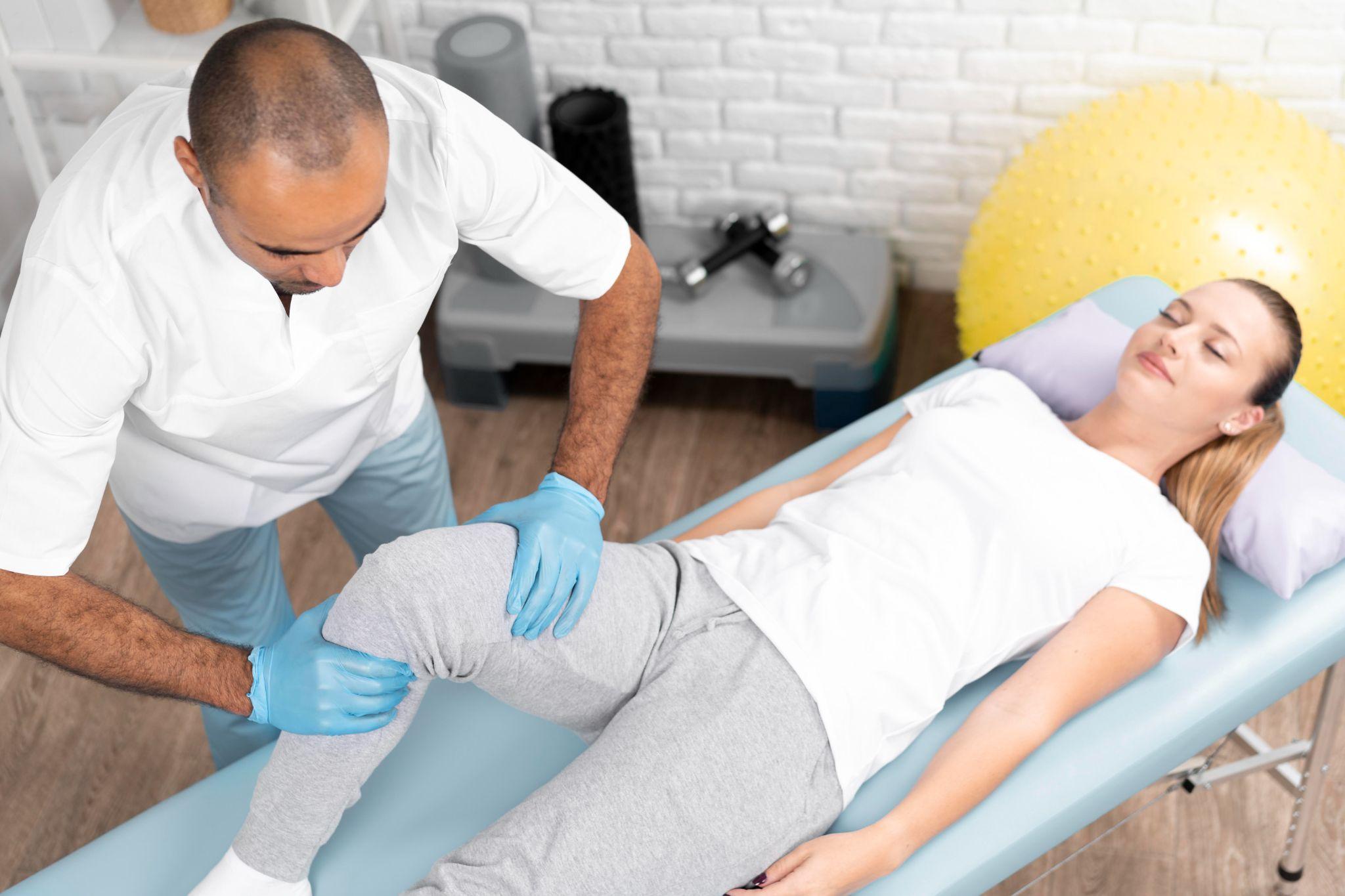
Hip pain is one of those complaints that sneaks up on people. It might start as a dull ache after a long walk or a twinge when you get out of the car. Most adults dismiss it, "I probably slept wrong" or "it'll go away on its own." But when that ache shows up again the next day, and the day after that, it's worth paying attention.
I've treated thousands of patients at my clinic in Noida who came in only after hip pain started disrupting their sleep, their commute, or their ability to play with their grandchildren. In most cases, the problem had been building for months, sometimes years, before they walked through my door. Early evaluation almost always leads to better outcomes.
Hip pain can stem from the joint itself, the muscles and tendons surrounding it, or even from problems in the lower spine. Getting the right diagnosis is the first step toward getting lasting relief.
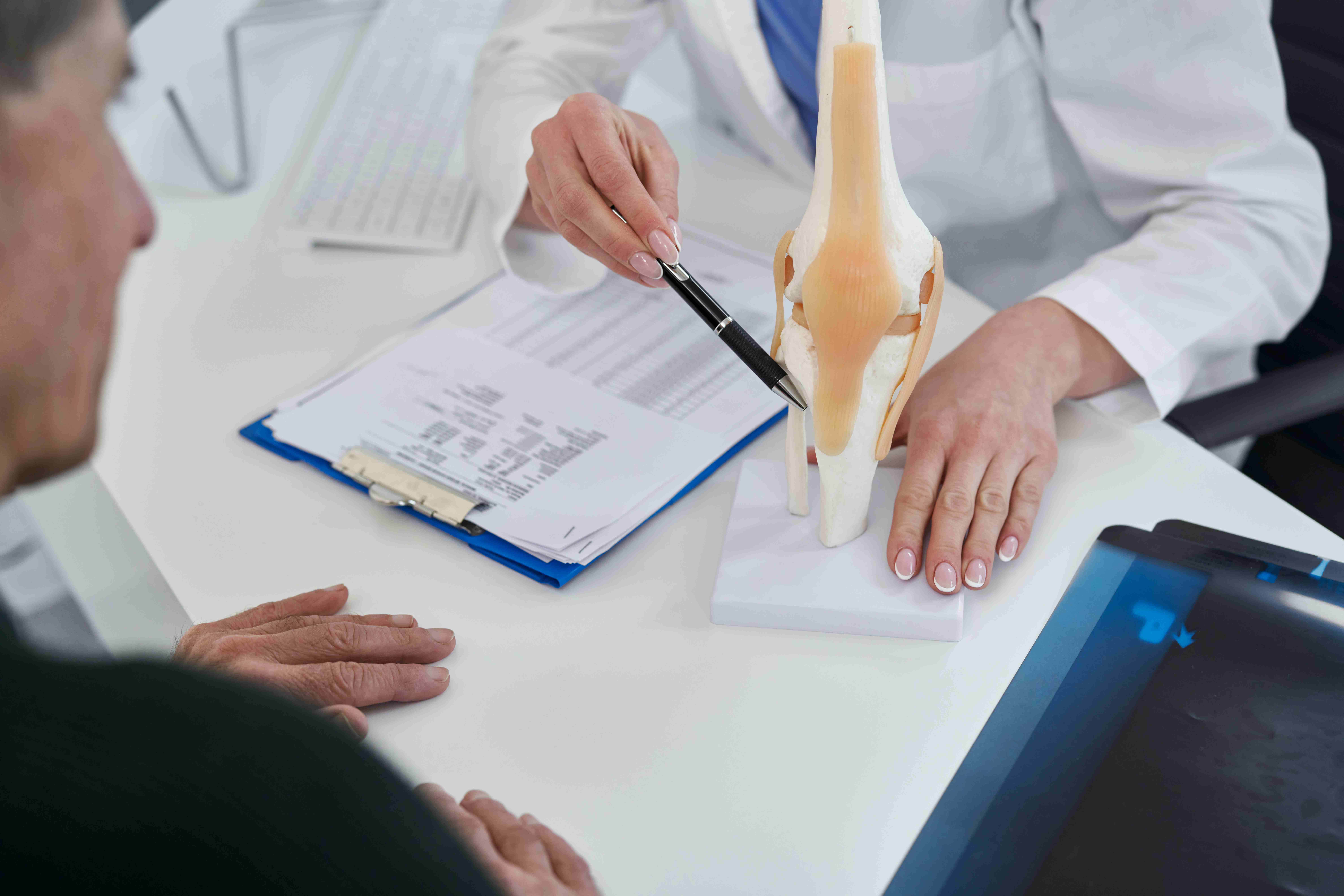
How the Hip joint works, and Why It's vulnerable
The hip is a ball-and-socket joint. The "ball" is the femoral head — the rounded top of your thigh bone, and the "socket" is the acetabulum, a cup-shaped cavity in the pelvis. This design allows a wide range of motion: bending, rotating, walking, squatting.
Several structures work together to keep the joint functional:
- Articular cartilage, a smooth, slippery tissue covering the ball and socket, allowing frictionless movement
- Labrum — a ring of fibrocartilage that deepens the socket and adds stability
- Synovial fluid, lubricates the joint and nourishes the cartilage
- Ligaments and tendons, connect bone to bone and muscle to bone, providing structural support
- Bursae — fluid-filled sacs that reduce friction between tissues
Because the hip bears your full body weight with every step, it's subjected to enormous forces, up to 3 to 5 times your body weight during activities like running or climbing stairs. That sustained load makes the hip susceptible to wear, inflammation, and injury over time.
Common causes of Hip pain in adults
1. osteoarthritis
This is the most frequent cause of hip pain in adults over 40, and it's the diagnosis I make most often in my clinic. Osteoarthritis develops when the cartilage lining the joint surfaces gradually thins and roughens. Without that smooth covering, bones start grinding against each other.
Symptoms typically include:
- Dull, aching pain in the groin or outer hip
- Morning stiffness lasting 20–30 minutes
- Pain that worsens after prolonged sitting or walking
- A grinding or crunching sensation during movement
- Gradual loss of range of motion, difficulty putting on socks or shoes
Osteoarthritis doesn't appear overnight. It progresses through stages. In early stages, X-rays may show only mild joint space narrowing. By the time a patient has bone-on-bone contact, they're often dealing with constant pain and significant stiffness. That's why catching it early matters — physiotherapy, weight management, and targeted exercises can slow the progression considerably.
2. muscle strain or tendon injury
The hip is surrounded by powerful muscle groups, the hip flexors, adductors, gluteal muscles, and hamstrings. Any of these can be strained through sudden movements, overuse, or inadequate warm-up before exercise.
This type of hip pain:
- Comes on suddenly after a specific activity, lifting, sprinting, lunging
- Feels sharp or pulling during movement
- Improves with rest but returns when you resume the activity
- May cause tenderness when you press the affected area
Mild strains typically recover within 2–4 weeks with rest, ice, and gentle stretching. Moderate tears may need 6–8 weeks and guided physiotherapy. If the pain persists beyond that window, imaging (usually an MRI) is warranted to rule out a more serious tear.
3. bursitis (Trochanteric bursitis)
The greater trochanter is the bony prominence you can feel on the outside of your hip. A bursa sits over it, cushioning the bone from overlying tendons and muscles. When that bursa becomes inflamed — from repetitive friction, prolonged standing, or a direct fall, it causes trochanteric bursitis.
Signs to watch for:
- Burning or aching pain on the outer hip
- Pain that worsens when lying on the affected side at night
- Tenderness when pressing over the bony prominence
- Increased discomfort when climbing stairs or getting up from a chair
Bursitis tends to respond well to rest, anti-inflammatory medication, and physiotherapy. In stubborn cases, a corticosteroid injection into the bursa can provide relief within a few days. I typically recommend this only after 4–6 weeks of failed conservative treatment.
4. sciatica (Referred pain from the spine)
Not all hip pain originates in the hip. This is something patients are often surprised to learn. When the sciatic nerve gets compressed or irritated in the lower spine, usually by a herniated disc or bone spur — the pain radiates down through the buttock and into the hip and leg.
Sciatic hip pain typically presents as:
- Shooting or electric pain that travels from the low back through the buttock to the leg
- Tingling, numbness, or a "pins and needles" sensation
- Pain that worsens with prolonged sitting or bending forward
- Weakness in the leg or foot in severe cases
Distinguishing sciatica from a true hip joint problem requires careful clinical examination. I often use specific provocative tests, the straight leg raise, FABER test, and internal rotation testing, to pinpoint whether the hip joint or the spine is the source. An MRI of the lumbar spine and hip may both be needed.

Medical illustration showing sciatic nerve pain radiating from lower back to leg
5. Hip labral tear
The labrum is a ring of tough cartilage that lines the rim of the hip socket. It deepens the socket, improves stability, and creates a seal that keeps synovial fluid inside the joint. A tear in the labrum can result from sports injuries (especially those involving twisting), structural abnormalities like hip impingement (femoroacetabular impingement, or FAI), or gradual degeneration.
Symptoms of a labral tear:
- Deep pain in the groin or front of the hip
- A clicking, catching, or locking sensation during movement
- Pain during hip rotation — turning the leg inward or outward
- Stiffness after sitting for long periods
Labral tears are often missed on standard X-rays. An MRI arthrogram, where contrast dye is injected into the joint before scanning, is the most reliable diagnostic tool. Treatment ranges from physiotherapy and activity modification in mild cases to arthroscopic surgery for tears that cause persistent mechanical symptoms.
6. Hip fractures
Hip fractures are most common in elderly individuals, particularly those with osteoporosis. A weakened bone can fracture from something as minor as a stumble or a misstep. In younger adults, hip fractures usually result from high-energy trauma — road accidents or falls from a height.
Warning signs:
- Sudden, severe pain after a fall
- Inability to bear weight on the affected leg
- The leg appears shorter or rotated outward
- Swelling and bruising around the hip
Hip fractures are surgical emergencies. Delayed treatment significantly increases the risk of complications, including blood clots, pneumonia, and pressure sores. Most hip fractures require surgical fixation with screws, plates, or, in elderly patients with displaced fractures, a partial or total hip replacement.
7. avascular necrosis (AVN)
Avascular necrosis occurs when the blood supply to the femoral head is disrupted. Without adequate blood flow, bone cells die and the bone gradually collapses. AVN has become increasingly recognized in India, and I've seen a noticeable uptick in cases over the past several years.
Risk factors include:
- Long-term or high-dose corticosteroid use (including during post-COVID treatment)
- Excessive alcohol consumption
- Previous hip injury or dislocation
- Sickle cell disease
- Radiation therapy
AVN is staged from I to IV based on severity. Early stages (I and II) may respond to core decompression — a procedure that drills small channels into the bone to encourage new blood vessel growth. By stage III or IV, when the femoral head has collapsed, hip replacement becomes the standard treatment.
Red-Flag symptoms, when to seek urgent care
Most hip pain isn't an emergency. But certain symptoms demand prompt evaluation:
- Pain lasting more than 2–3 weeks without improvement
- Difficulty walking or standing from a seated position
- Night pain that wakes you from sleep
- Swelling, redness, or warmth around the joint, could indicate infection
- Fever combined with joint pain — a possible sign of septic arthritis, which requires emergency treatment
- Severe pain after a fall, especially in anyone over 60
- Sudden inability to bear weight
If any of these apply, don't wait. See an orthopedic specialist.
How Hip pain Is diagnosed
When a patient comes to me with hip pain, my assessment follows a systematic approach:
History: When did the pain start? Where exactly do you feel it? Does it radiate? What makes it worse or better? Have you had any injuries, surgeries, or chronic illnesses?
Physical examination: I test range of motion, strength, and specific clinical signs. The FABER test (flexion, abduction, external rotation) helps identify hip joint pathology. The log roll test checks for intra-articular problems. Tenderness over the greater trochanter suggests bursitis.
Imaging:
- X-rays, first-line investigation; reveals fractures, arthritis, joint space narrowing, AVN changes
- MRI, evaluates soft tissues including the labrum, tendons, muscles, and early AVN
- Ultrasound — useful for assessing bursitis and guiding injections
- Blood tests, ordered when infection, rheumatoid arthritis, or gout is suspected (CBC, ESR, CRP, uric acid, rheumatoid factor)
Treatment options
Non-Surgical treatment
The majority of hip conditions improve with conservative management:
- Activity modification, reducing activities that aggravate pain while staying mobile
- Physiotherapy — targeted exercises to strengthen hip stabilizers and improve flexibility
- Anti-inflammatory medications, short courses of NSAIDs (like ibuprofen or naproxen) to control pain and swelling
- Weight management, every kilogram of excess body weight adds roughly 3–5 kg of force on the hip joint during walking
- Corticosteroid or hyaluronic acid injections — for targeted relief in cases of bursitis, arthritis, or labral tears
Surgical treatment
When conservative treatment fails or the condition is advanced, surgery may be necessary:
- Arthroscopy, a minimally invasive procedure using small incisions and a camera; used for labral repairs, removal of loose bodies, and treatment of hip impingement
- Fracture fixation, screws, plates, or nails to stabilize broken bones
- Core decompression — for early-stage AVN
- Total hip replacement, the gold standard for end-stage arthritis or AVN with femoral head collapse; modern prostheses last 20–25 years in most patients
Recovery after hip replacement typically involves 2–3 days of hospital stay, walking with support within 24–48 hours of surgery, and a return to normal activities within 6–12 weeks.

Orthopedic surgeons performing hip surgery in an operation theater
Practical steps to protect your hips
You don't need a gym membership to take care of your hips. These habits make a real difference:
- Maintain a healthy weight, even modest weight loss reduces joint stress significantly
- Strengthen your hip and core muscles — squats, bridges, clamshells, and side-lying leg raises help stabilize the joint
- Stretch your hip flexors daily, especially if you sit for long hours at work
- Avoid sudden, explosive movements without proper warm-up
- Ensure adequate Vitamin D and calcium intake, both are essential for bone and cartilage health
- Wear proper footwear — shoes with good cushioning reduce impact on the hips during walking and running
When to See an orthopedic specialist
If hip pain is interfering with your daily life, your ability to walk, work, sleep, or exercise, waiting only makes things harder. The longer a problem goes untreated, the more damage accumulates, and the more limited your treatment options become.
At my practice at KDSG Hospital, Noida, we offer thorough diagnostic evaluation and individualized treatment plans for hip pain, arthritis, fractures, AVN, sports injuries, and joint disorders. Most patients with hip problems can return to full activity with the right treatment at the right time.
If you've been dealing with persistent hip pain, schedule a consultation so we can find the cause and get you moving comfortably again.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.