Foot And Ankle Pain You Should Not Ignore - When To See An Orthopedic Specialist In Noida

Medical illustration highlighting the plantar fascia ligament and heel bone affected in plantar fasciitis.
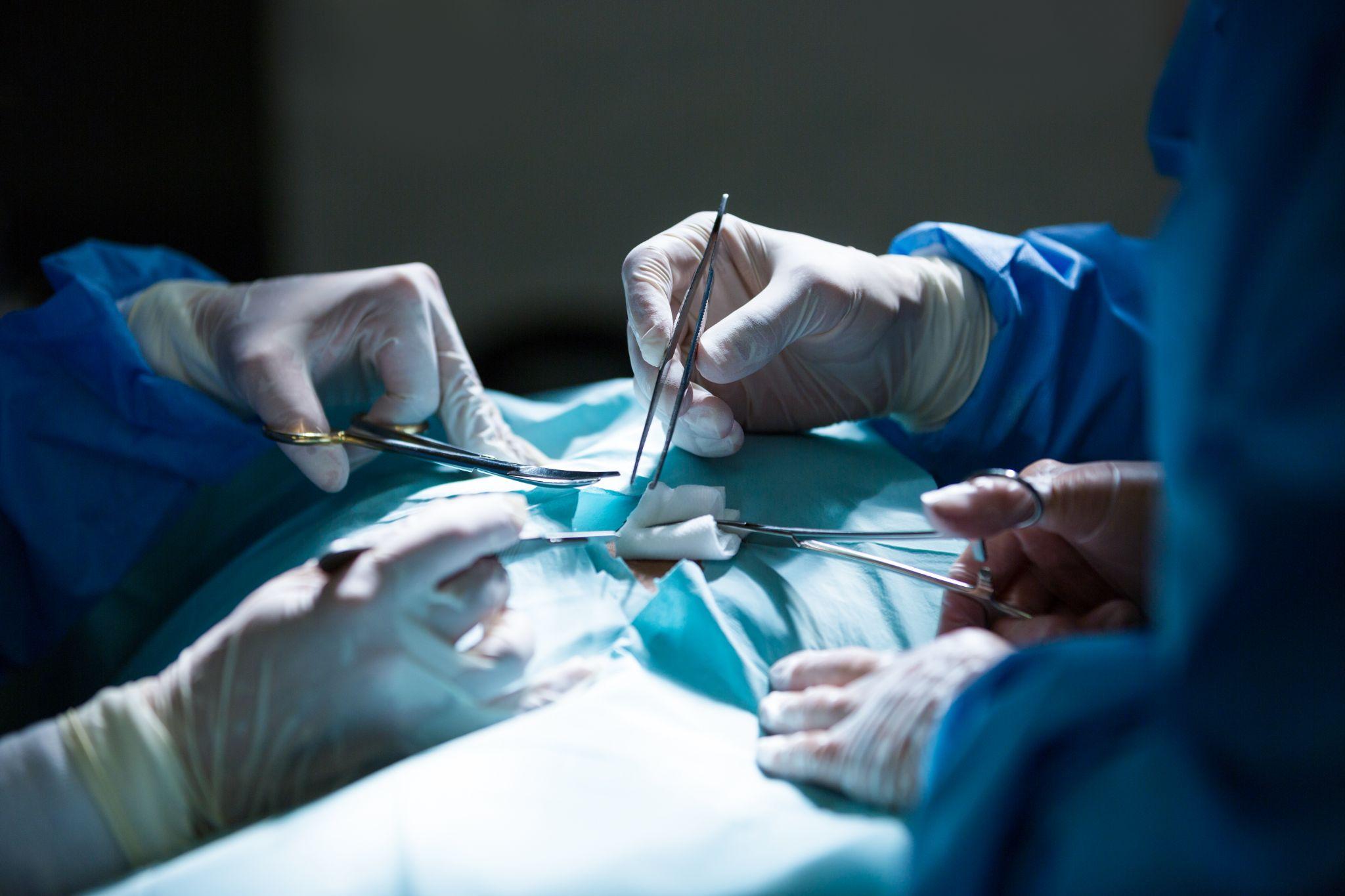
Most people have experienced the occasional sore ankle after a long walk or foot pain after standing all day at work. That kind of discomfort is normal and usually goes away with rest in a day or two. But there is a different category of foot and ankle pain; pain that persists, that gets progressively worse, that keeps coming back after the same activities, or that changes the way you walk. This type of pain is your body signalling something structural that home remedies are unlikely to fix.
The foot and ankle are complex structures. Each foot contains 26 bones, 33 joints, and over 100 tendons, muscles, and ligaments. When something goes wrong in this system, whether through injury, overuse, or a degenerative process, the effects extend upward into the knee, hip, and lower back, because the way we compensate for foot pain changes how we load every joint above it. This guide covers the most common foot and ankle conditions, the warning signs that warrant specialist attention, and the treatment options available to patients in Noida and Greater Noida.
Common Foot And Ankle Conditions
Foot and ankle conditions can affect mobility, balance, and daily comfort, making early diagnosis and proper treatment essential for maintaining an active lifestyle.
1. Ankle Sprains And Ligament Injuries
Ankle sprains are among the most common musculoskeletal injuries in India, affecting people across age groups, from school-level footballers to working adults who step off a pavement incorrectly. The lateral ligaments (on the outer side of the ankle) are most commonly affected.
A sprain that is managed well with rest, ice, compression, elevation, and early physiotherapy typically heals within two to six weeks. But the problem is that many people walk off with an ankle sprain without proper treatment, and the ligaments heal loosely or incompletely. This leads to chronic ankle instability, a condition where the ankle repeatedly gives way with minimal provocation. Over the years, repeated sprains cause cumulative damage to the cartilage and the joint itself, eventually leading to ankle arthritis.
If your ankle has been sprained more than once or if it still feels unstable months after an injury, a specialist evaluation is warranted.
2. Achilles Tendinitis And Tendinopathy
The Achilles tendon connects the calf muscles to the heel bone. Overuse from sudden increases in running distance, wearing unsupportive footwear, or sustained activity on hard surfaces inflames or degenerates this tendon, causing pain along the back of the ankle and stiffness in the morning.
Mild Achilles tendinitis responds well to physiotherapy, load management, and orthotics. Persistent or severe cases or those involving a partial or complete tendon rupture require specialist assessment. A complete Achilles rupture (sudden sharp pain at the back of the ankle, often feeling like being kicked) is a surgical emergency that requires urgent management.
3. Plantar Fasciitis
This is one of the most common causes of heel pain in adults. The plantar fascia is a band of tissue running along the bottom of the foot from the heel to the toes. When it becomes inflamed, typically from prolonged standing, sudden increases in activity, poor footwear, or tight calf muscles, it causes sharp heel pain, classically worst with the first few steps in the morning.
Most cases of plantar fasciitis resolve with physiotherapy, stretching, supportive footwear, and occasionally steroid injections. Cases that persist beyond six months despite adequate conservative treatment may require further intervention.
4. Ankle Arthritis
Ankle arthritis is less common than knee or hip arthritis, but it is particularly debilitating because the ankle bears the full weight of the body during every step. It often follows significant trauma, a major ankle fracture that was not perfectly reconstructed, or years of repetitive sprains with ligamentous instability.
The primary symptoms are pain with weight-bearing activity, stiffness (especially in the morning), swelling, and a gradual reduction in ankle range of motion. As the arthritis progresses, even short-distance walking becomes painful. Treatment ranges from conservative management (orthotics, physiotherapy, anti-inflammatory medication, injections) to surgical options, including ankle arthroscopy to debride the joint or, in severe cases, ankle fusion or ankle replacement.
5. Stress Fractures

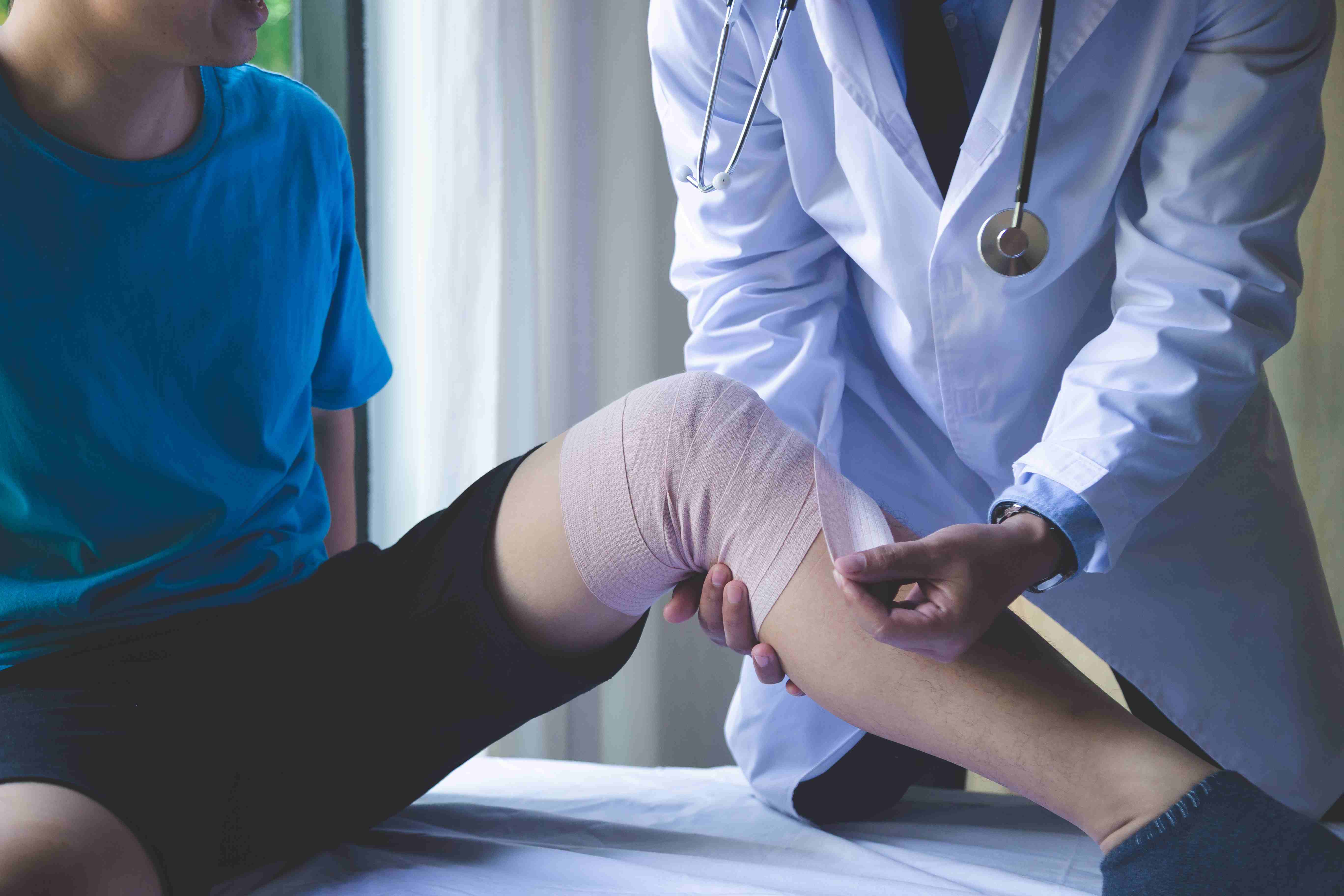
A close-up shot of a female doctor examining the fractured foot of a male patient with a blue casket on it.
Stress fractures are tiny cracks in the bone, typically caused by repetitive loading rather than a single traumatic event. In the foot, the metatarsal bones are most commonly affected. Stress fractures are particularly common in athletes who increase their training volume quickly, and in patients with reduced bone density (osteoporosis).
The hallmark is localised, point-specific tenderness that worsens with activity and improves with rest. X-rays may appear normal in early stages; MRI is the definitive investigation. Untreated stress fractures can progress to complete fractures, which is why persistent, activity-related foot pain in an athlete should always be assessed rather than dismissed.
6. Flat Feet And High Arches
Both extremes of foot arch can cause pain and affect the biomechanics of the entire lower limb. Flat feet (pes planus) can strain the posterior tibial tendon, leading to progressive arch collapse in adults, a condition called adult-acquired flatfoot deformity. High-arched feet (pes cavus) place excessive stress on the outer ankle and heel, predisposing patients to stress fractures and lateral ankle instability. These structural conditions rarely require surgery in their early stages but benefit significantly from properly fitted orthotics, physiotherapy, and footwear guidance.
Warning Signs That Require Urgent Specialist Attention
Some foot and ankle symptoms should not wait for a scheduled appointment. Seek urgent evaluation from an orthopedic specialist in Noida or Greater Noida if you experience:
- Sudden, severe pain in the heel or back of the ankle following a sprint or jump (possible Achilles rupture).
- Inability to bear weight on the foot after an injury.
- Visible deformity of the foot or ankle following trauma.
- A popping or snapping sensation at the time of injury, followed by immediate swelling.
- Numbness or tingling in the foot that is persistent or worsening (possible nerve involvement).
- Swelling that does not reduce with elevation and rest over several days.
- Open wounds on the foot in patients with diabetes infection can progress rapidly and have serious consequences.
When To See A Foot And Ankle Orthopedic Specialist (Non-Urgent)
See an orthopedic specialist in Noida for foot or ankle pain if:
- Pain has persisted for more than two weeks without improvement despite rest.
- The ankle feels unstable or has given way more than once.
- Swelling is present that does not respond to basic rest and elevation.
- Pain is affecting your walking pattern, sleep, or daily activities.
- You have tried over-the-counter pain relief without adequate benefit.
- An MRI or X-ray has shown a structural abnormality that needs interpretation.
Early assessment prevents minor problems from progressing into complex, harder-to-treat conditions. Patients who wait months for ankle instability to resolve on its own often develop cartilage damage that would not have occurred with earlier intervention.
Foot And Ankle Treatment At Dr. Ankur Singh's Clinic In Noida

A runner sitting on the ground holding his foot, showing symptoms of plantar fasciitis-related pain.
Dr. Ankur Singh specialises in foot and ankle joint surgery as part of his comprehensive orthopedic practice at Noida and Greater Noida. Services include:
- Clinical evaluation and MRI/X-ray assessment of foot and ankle injuries.
- Physiotherapy guidance and conservative management planning.
- Arthroscopic ankle surgery for cartilage injuries, loose bodies, and ankle impingement.
- Surgical management of chronic ankle instability.
- Management of ankle and foot arthritis.
If you have been managing foot or ankle pain in Noida or Greater Noida and are not getting adequate relief with rest and home treatment, a specialist assessment will identify what is actually happening and what the best management approach looks like. To book a consultation, call the number listed on this website.
Frequently Asked Questions
1. Can ankle sprains heal without physiotherapy?
Minor sprains with intact ligament function often heal with basic rest and time. However, sprains involving significant ligament laxity or repeated sprains need physiotherapy to restore proprioception and strength. Without this, the ankle remains at high risk of re-injury.
2. Is surgery always needed for ankle arthritis?
No. Many patients with mild to moderate ankle arthritis do well with conservative management, orthotics, physiotherapy, activity modification, and injections. Surgery (ranging from arthroscopy to fusion or replacement) is considered when conservative measures no longer control symptoms adequately.
3. Can plantar fasciitis become permanent?
Most cases of plantar fasciitis resolve within 12 months with proper management. Chronic cases (lasting beyond this) are less common and may require more targeted interventions. Persistent plantar fasciitis rarely requires surgery but does need structured treatment rather than just waiting.
4. Is foot and ankle orthopedic care available in Greater Noida?
Yes. Dr. Ankur Singh sees and treats foot and ankle conditions at KDSG Superspeciality Hospital in Greater Noida, serving patients from across the Delhi-NCR region.
Dr. Ankur Singh | Best Orthopedic Surgeon in Noida | Foot and Ankle Joint Surgery | Ankle Arthroscopy | KDSG Superspeciality Hospital, Greater Noida
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.