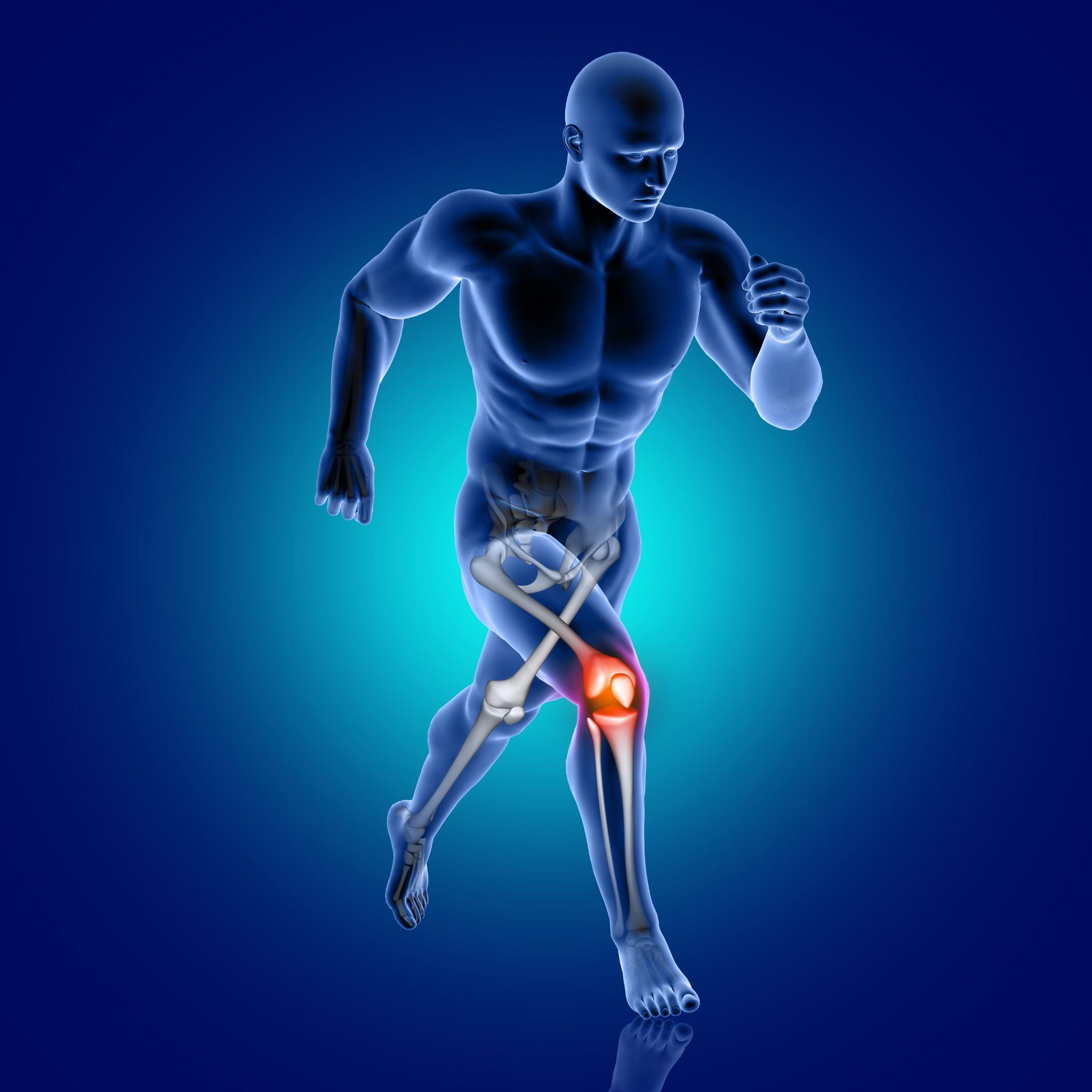
Why ignoring early joint pain often leads to long-Term damage

Elderly man experiencing knee joint pain due to ignoring it at first
A twinge in your knee when you take the stairs. Stiffness in your fingers first thing in the morning. A dull ache in the shoulder that lingers after a long day at your desk. Most people brush these off. They assume it's fatigue, aging, or something that'll resolve on its own with a few days of rest.
That assumption can be costly.
In my 15+ years of orthopedic practice, I've seen a pattern repeat itself hundreds of times: a patient comes in with advanced cartilage loss, chronic stiffness, or a joint that barely functions, and when I ask how long they've had symptoms, the answer is almost always "years." Early joint pain is rarely random. It's the body's alarm system, and it fires for a reason.
The difference between a joint that heals fully and one that deteriorates permanently often comes down to how early you act.
What early joint pain actually means
Joint pain in its earliest stage is usually mild. You might notice it only after a run, a long walk, or sitting cross-legged for too long. It fades with rest. You can still do everything you normally do. And that's exactly why people ignore it, because it doesn't seem like a real problem yet.
Early signs that deserve attention:
- Mild discomfort after physical activity — walking, exercising, standing for extended periods
- Morning stiffness that lasts 10–30 minutes and eases with movement
- Occasional swelling around a joint, especially after use
- A rough or grating sensation during movement (called crepitus)
- Slight loss of flexibility, you can't bend or straighten the joint quite as far as you used to
At this stage, the damage inside the joint is minimal. The cartilage may have microscopic wear. The synovial membrane might be mildly inflamed. With the right intervention, targeted exercises, activity modification, anti-inflammatory treatment — these changes are largely reversible.
The window doesn't stay open forever.

Senior man suffering from lower back stiffness.
Why the body can't "Push through" joint damage
Joints are precision-engineered structures. Each one relies on a specific combination of articular cartilage (the smooth, shock-absorbing surface), synovial fluid (the lubricant), ligaments (the stabilizers), tendons (the connectors), and surrounding muscles (the protectors). When any of these components is stressed beyond its capacity, the joint signals you with pain or stiffness.
Pain is a diagnostic signal, not the disease itself
Too many people treat pain as the enemy. They pop a painkiller and carry on. But pain is information, it's telling you that something inside the joint is under strain. Suppressing the signal doesn't stop the underlying process. It just hides it.
Compensation injuries: one problem becomes three
When a joint hurts, your body instinctively adapts. You shift weight off a painful knee. You rotate your shoulder differently to avoid a sore spot. You change your walking pattern to protect a stiff hip.
These compensations feel like solutions, but they create secondary problems. The opposite knee starts taking extra load. The lower back tightens from an altered gait. Within months, what started as pain in one joint has spread to two or three areas. I see this cascade in my clinic regularly, a patient comes in with knee pain, and on examination, their hip, lower back, and ankle are all compromised because they've been walking abnormally for a year.
How untreated joint pain progresses — the four stages
Joint deterioration follows a predictable trajectory. Understanding these stages helps explain why early intervention matters so much.
Stage 1: inflammation and micro-damage (weeks to months)
The initial insult comes from overuse, poor biomechanics, a minor injury, or weak stabilizing muscles. The synovial membrane becomes inflamed. Cartilage develops microscopic surface irregularities, not visible on X-rays, but detectable on MRI in some cases. Pain is intermittent and mild. Most patients don't seek help at this stage.
What works at this stage: Rest, physiotherapy, anti-inflammatory medication, biomechanical correction, strengthening exercises. Response rates are excellent, upwards of 85–90% of patients improve without any further intervention.
Stage 2: cartilage wear and persistent stiffness (months to 1–2 years)
If the inflammation isn't addressed, cartilage begins to thin. Cartilage has extremely limited self-repair capacity because it has almost no blood supply. Damage accumulates gradually. Stiffness becomes a daily occurrence rather than an occasional nuisance. Pain lasts longer after activity and starts appearing even during routine tasks — climbing stairs, squatting, gripping objects.
What works at this stage: Structured physiotherapy, joint-specific exercises, weight management, and in some cases, intra-articular injections (corticosteroids or viscosupplementation) to reduce inflammation and improve joint lubrication.
Stage 3: structural joint damage (1–5 years without treatment)
The cartilage is significantly eroded. Bones may start to contact each other directly. The joint space visible on X-rays narrows measurably. Osteophytes (bone spurs) can form as the body tries to stabilize the damaged joint. Swelling becomes persistent. Osteoarthritis is typically diagnosed at this point.
What works at this stage: Pain management, advanced physiotherapy, activity modification, bracing or orthotics, and for some patients, surgical options like arthroscopy or osteotomy to realign the joint.
Stage 4: chronic pain and functional loss (years of neglect)
By this stage, the joint is severely compromised. Constant pain. Marked restriction of movement. Muscle wasting around the joint from prolonged disuse. Basic tasks, walking across a room, getting in and out of a car, buttoning a shirt, become difficult or impossible. Joint replacement surgery is often the only remaining option that can restore function.
The real consequences of delayed treatment
1. irreversible cartilage loss
Once cartilage is significantly damaged, it doesn't grow back. There are no medications, supplements, or therapies that can regenerate large areas of lost cartilage. Prevention and early treatment aren't just preferable — they're the only reliable strategy.
2. higher risk of osteoarthritis
Osteoarthritis doesn't appear out of nowhere. It develops from years of untreated joint stress, unresolved inflammation, or biomechanical imbalances. A joint that's been sore for two years is far more likely to progress to arthritis than one that was treated at the two-week mark.

Elderly man holding knee affected by arthritis and joint inflammation
3. loss of independence
When joints can no longer support daily activities, dependence on others increases. Climbing stairs, getting out of bed, walking to the market, lifting a bag of groceries, these aren't luxuries. They're the activities that define independent living. Losing them affects everything.
4. mental health impact
Chronic joint pain doesn't just affect the body. It disrupts sleep, limits social activity, and erodes confidence. Patients with untreated chronic musculoskeletal pain report higher rates of anxiety, depression, irritability, and social withdrawal. The connection between persistent pain and mental health deterioration is well-documented and often underestimated.
5. financial burden
Late-stage joint problems are expensive to treat. A total knee replacement costs significantly more, both financially and in recovery time — than a course of physiotherapy and lifestyle modification started early. I always tell my patients: spending time and effort on prevention now saves you from spending far more on treatment later.
Why painkillers alone make things worse
Reaching for an over-the-counter painkiller when joints ache is understandable. NSAIDs (ibuprofen, diclofenac) and paracetamol provide real relief. But they mask pain, they don't treat the cause.
The dangers of relying on painkillers:
- Inflammation continues unchecked, you feel better, but the joint damage progresses silently
- Overuse injury worsens — without pain to limit you, you push the joint harder than it can handle
- Organ damage from chronic use, prolonged NSAID use can cause gastric ulcers, kidney impairment, and cardiovascular risks; paracetamol overuse can damage the liver
- Delayed diagnosis, painkillers can obscure symptoms for months or years, during which the condition advances from treatable to irreversible
Painkillers have a place in joint care — as part of a treatment plan, not as the entire plan. The priority should always be identifying and addressing the root cause.
Who faces the highest risk?
Joint damage isn't limited to the elderly. In my practice, I'm seeing more patients in their 30s and 40s with early-stage joint problems than ever before. Several groups face elevated risk:
- Desk workers and sedentary individuals, prolonged sitting weakens the muscles that support joints, particularly the knees and hips
- People with poor posture, forward head posture, rounded shoulders, and slumped sitting all increase abnormal load on joints
- Those carrying excess weight — every extra kilogram adds 3–5 kg of force on the knee joint during walking
- Athletes and physically active individuals, repetitive stress on the same joints (runners' knees, cricketers' shoulders, tennis elbows) causes cumulative wear
- Older adults with declining muscle mass, sarcopenia reduces the muscular scaffolding that protects joints
- People with a family history of arthritis — genetic predisposition increases susceptibility
When should You take action?
Don't wait for pain to become unbearable. The earlier you get assessed, the more options you have.
Consult an orthopedic specialist if:
- Joint pain persists beyond 2 weeks despite rest
- Stiffness is present daily, especially in the mornings
- Swelling comes and goes without clear injury
- Pain limits your ability to perform routine activities, walking, climbing stairs, gripping, bending
- You're taking painkillers more than 2–3 times per week for joint pain
- You notice a change in your walking pattern or posture
An early evaluation typically involves a clinical examination, possibly X-rays or an MRI, and, most critically — a clear plan tailored to your specific condition.
What early treatment actually involves
Treatment caught at stage 1 or 2 is straightforward and highly effective:
- Physiotherapy, targeted strengthening and flexibility exercises prescribed by a trained therapist
- Biomechanical correction, addressing gait abnormalities, flat feet, or muscle imbalances that contribute to joint stress
- Weight management — even 5% body weight loss can reduce knee pain by 20–30%
- Activity modification, not stopping activity, but modifying it to reduce harmful load on affected joints
- Anti-inflammatory treatment, short-term medication to calm active inflammation
- Posture correction — ergonomic adjustments at your workstation, sleeping position, and daily movement patterns
- Nutritional support, ensuring adequate calcium, vitamin D, and protein for bone and cartilage maintenance
None of these are invasive. None require surgery. And when started early, they can prevent you from ever needing surgery.
Building joint-Healthy habits for the long term
Daily practices that protect your joints:
- Stay active with low-impact exercise, swimming, cycling, walking, yoga; these strengthen the muscles around joints without excessive wear on cartilage
- Maintain healthy body weight — one of the single most effective things you can do for your knees and hips
- Stretch before and after physical activity, cold muscles and tight tendons increase injury risk
- Avoid sustained awkward postures, don't sit cross-legged on the floor for hours, don't hunch over your phone, don't sleep on a sagging mattress
- Address pain early — treat discomfort as a signal, not an inconvenience
- Get periodic check-ups, especially after 40, or if you have a family history of arthritis or osteoporosis
Final word
Early joint pain isn't something to "tough out." It's a signal from your body that a process has started, one that's manageable now but won't be if left unchecked for years.
I've treated patients who came in at stage 1 and walked out with a simple exercise plan. I've also treated patients who came in at stage 4 and needed a joint replacement. The difference between these outcomes is almost always the same: timing.
If you've been noticing joint pain, stiffness, or swelling that won't go away, an evaluation with a qualified orthopedic specialist can catch the problem while it's still easily treatable. At my clinic at KDSG Hospital, Noida, we focus on accurate early diagnosis and evidence-based treatment to help patients avoid long-term damage and stay active for life.
Don't let a small ache become a permanent problem. Get it checked.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.