What Is frozen shoulder

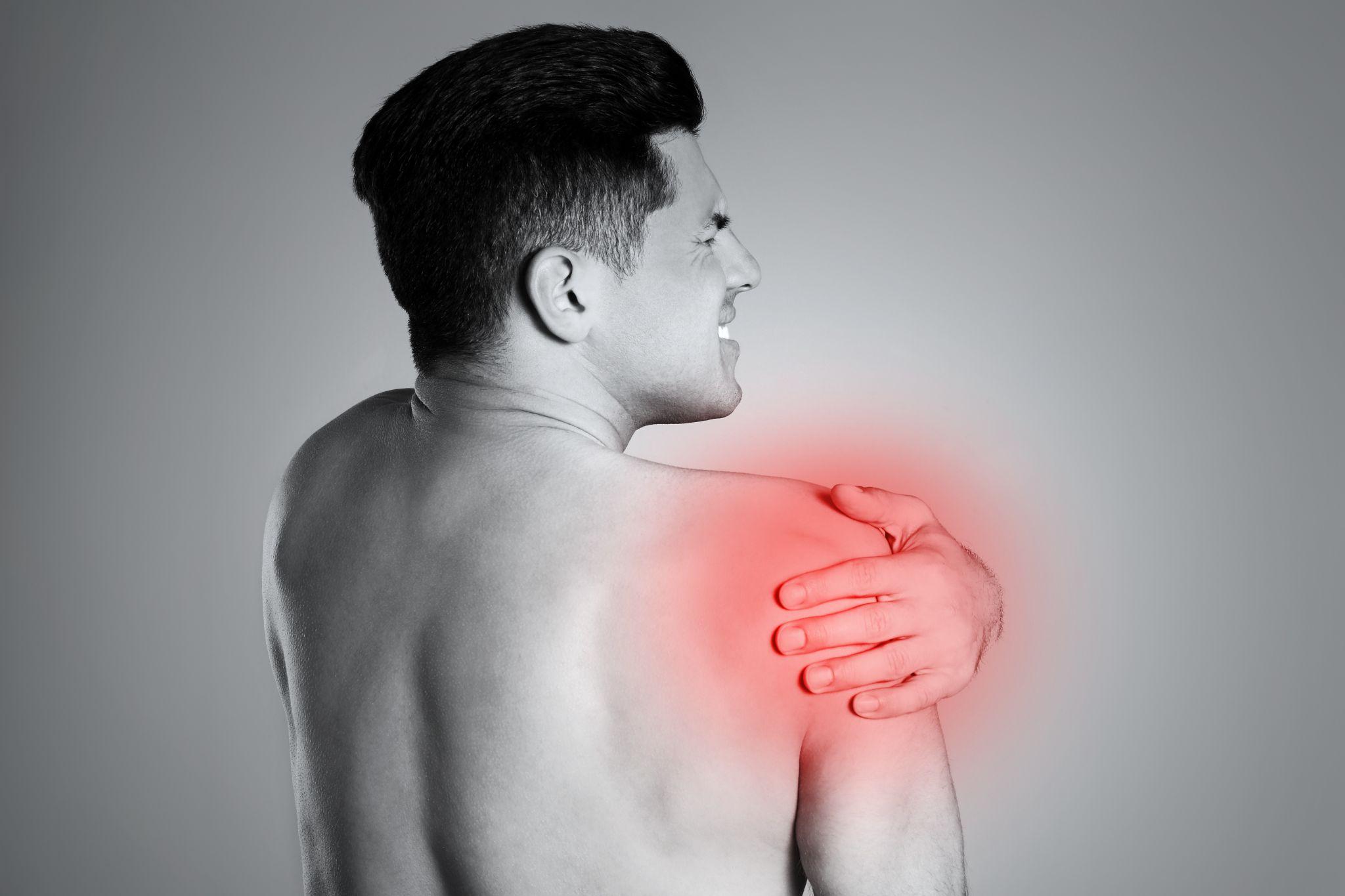
A man holding his shoulder in pain due to frozen shoulder.
Frozen shoulder, or Adhesive Capsulitis, as we call it in medicine, is one of the most frustrating conditions I treat at my clinic. Patients walk in unable to comb their hair, hook a bra strap, or reach for a glass on a high shelf. The shoulder has essentially locked up. Pain is constant, sleep is disrupted, and daily life feels like a battle.
About 2 to 5 out of every 100 adults will develop frozen shoulder at some point. It creeps up slowly, sometimes without any obvious injury, and if it isn't addressed early, it can drag on for a year or even longer. I see at least 3–4 frozen shoulder cases every week at KDSG Superspeciality Hospitals, and the single biggest mistake patients make is waiting too long before seeking help.
What exactly is a frozen shoulder?
The shoulder joint is wrapped in a flexible tissue called the joint capsule. Think of it as a sleeve around the ball-and-socket joint. In a frozen shoulder, this capsule becomes inflamed, thickened and scarred. Bands of scar tissue (called adhesions) form inside the capsule, and the capsule itself shrinks. The result is pain plus severe stiffness — you can't move the shoulder yourself, and even someone else trying to move it for you meets resistance.
This is different from a rotator cuff tear, where the tendons are damaged but the capsule is intact. In my practice, patients often confuse the two because the pain location is similar. A proper clinical examination quickly tells them apart.
Frozen shoulder typically strikes between ages 40 and 60. Women are affected more often than men, roughly 60% of the cases I see are in women, particularly those going through perimenopause or early menopause. It usually hits one shoulder, but about 15–20% of patients eventually develop it on the other side too.
Common causes of frozen shoulder
The exact trigger isn't always clear. Many patients tell me, "Doctor, I didn't do anything, it just started hurting one day." That said, several known factors raise the risk significantly.
1. prolonged immobilization
Anytime the shoulder stays still for weeks, the capsule can start tightening. I commonly see this after:
- Arm or collarbone fractures treated with a sling
- Rotator cuff surgery or breast surgery
- Heart surgery (patients avoid moving that arm)
- Even a stroke affecting one side of the body
This is exactly why physiotherapy starts early after shoulder surgeries — to prevent the capsule from stiffening.
2. diabetes
This is a big one. Diabetic patients are roughly 2 to 5 times more likely to develop frozen shoulder compared to non-diabetics. In my clinic, I'd estimate nearly 30–40% of frozen shoulder patients also have diabetes (sometimes undiagnosed). The frozen shoulder in diabetic patients tends to be more stubborn and takes longer to resolve. If you have diabetes and notice shoulder stiffness creeping in, don't wait, get it checked early.
3. thyroid and hormonal disorders
Both hypothyroidism (underactive thyroid) and hyperthyroidism raise the risk. Hormonal shifts during menopause are another common trigger, which partly explains why women in their late 40s and 50s are so frequently affected.
4. autoimmune and inflammatory conditions
Rheumatoid arthritis, lupus and other autoimmune disorders can irritate the joint capsule over time. Chronic low-grade inflammation makes the capsule more prone to scarring.
5. postural strain and desk work
I tell my patients this often: prolonged hunching over a laptop, with rounded shoulders, puts the shoulder joint in a compressed position for hours. Over months and years, this can contribute to capsular tightness. It doesn't cause frozen shoulder on its own, but it creates the conditions for it.
Symptoms of frozen shoulder
The hallmark of frozen shoulder is a combination of pain and stiffness, not one or the other, but both. Here's what patients typically describe:
- A deep, dull ache inside the shoulder (not a sharp, stabbing pain)
- Difficulty raising the arm above shoulder height
- Can't reach behind the back — tucking in a shirt or fastening a bra becomes nearly impossible
- Stiffness that worsens at night, often waking you up
- Both active movement (you trying to move) and passive movement (someone else moving your arm) are restricted
- Pain that radiates down the upper arm but rarely goes below the elbow
One useful clue: if the pain goes all the way down to your hand or fingers, that's usually not frozen shoulder, it could be a cervical spine issue, and the diagnosis changes entirely.
The 3 stages of frozen shoulder
Frozen shoulder follows a predictable pattern of three stages. Understanding which stage you're in helps guide treatment.
1. freezing stage (The painful phase)
- Duration: 6 weeks to 9 months
- Pain is the dominant symptom. It starts mild and builds over weeks.
- Shoulder movement decreases gradually, you notice you can't reach as far as before.
- Night pain is worst during this stage. Lying on the affected side becomes very uncomfortable.
- Most patients first visit the doctor during this phase.
2. frozen stage (The stiff phase)
- Duration: 4 to 12 months
- Pain actually starts reducing — many patients feel relieved.
- But stiffness is now at its worst. The shoulder feels locked.
- Everyday tasks, wearing a pullover shirt, washing your hair, driving, become a real struggle.
- Range of motion can drop to less than 50% of normal.
3. thawing stage (Recovery phase)
- Duration: 6 months to 2 years
- Movement slowly starts returning.
- Pain continues to decrease.
- With consistent physiotherapy, most patients recover 80–90% of their range of motion. Full recovery is possible, but some patients retain a mild restriction that doesn't bother them functionally.
Without any treatment, the total cycle — from freezing to thawing, can last 18 months to 3 years. With proper treatment, this timeline can be shortened significantly.
How is frozen shoulder diagnosed?
In most cases, I can diagnose frozen shoulder through a clinical examination alone, no fancy tests needed. Here's what I look for:
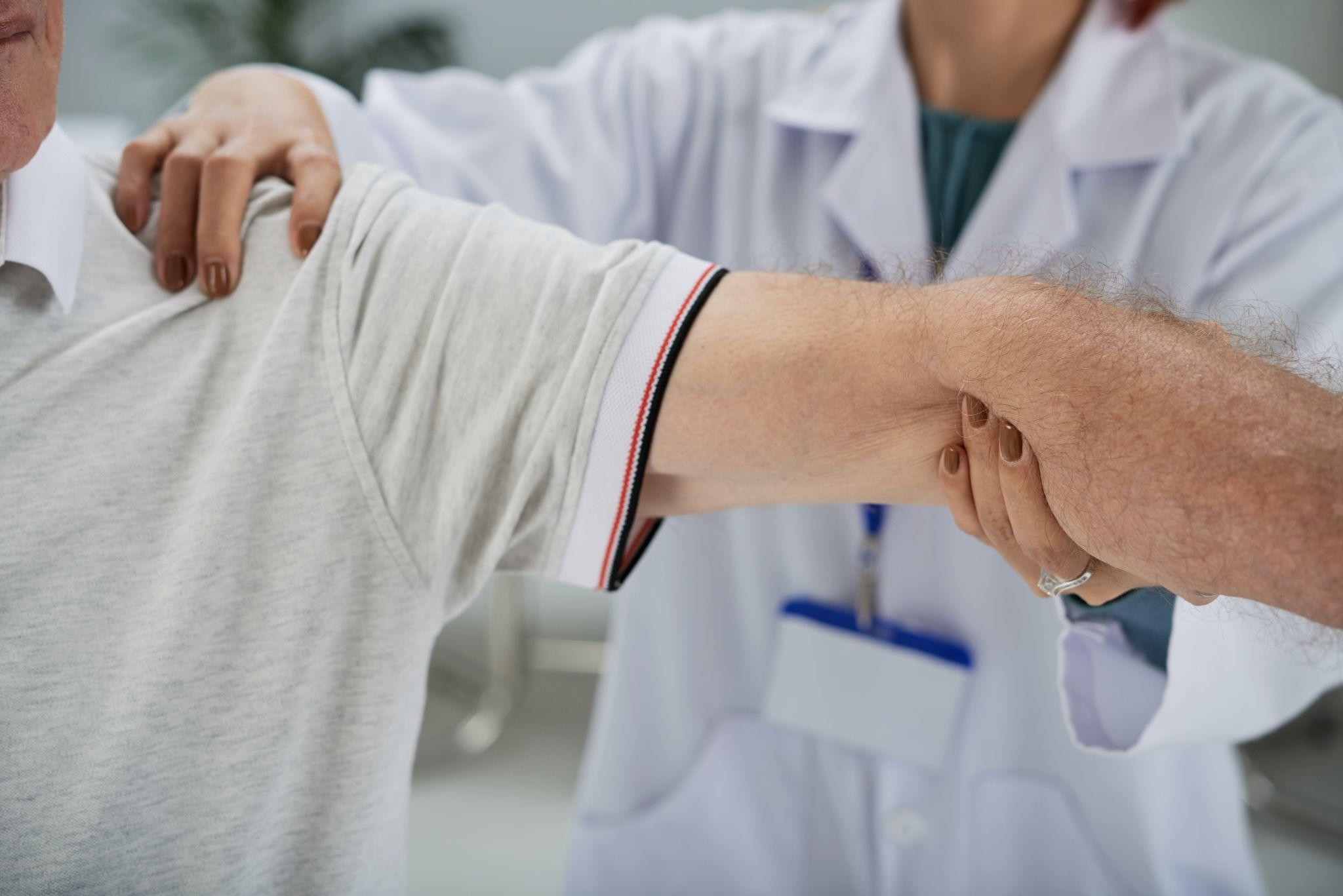
Physical examination: I check both active and passive range of motion. The key finding is a global restriction — the shoulder is stiff in all directions (forward flexion, abduction, and external rotation). External rotation (turning the arm outward) is usually the most restricted movement. If a patient can't rotate the arm outward even when I assist, frozen shoulder is very likely.
Medical history: I ask about diabetes, thyroid problems, recent injuries, and any period of immobilization.
Imaging tests are ordered mainly to rule out other conditions:
- X-ray, to check for arthritis, fractures or calcium deposits
- MRI, if I suspect a rotator cuff tear or labral injury alongside the frozen shoulder
- Ultrasound — occasionally used to assess the capsule thickness
Blood tests may be done to check for diabetes or thyroid dysfunction if these haven't been screened recently.
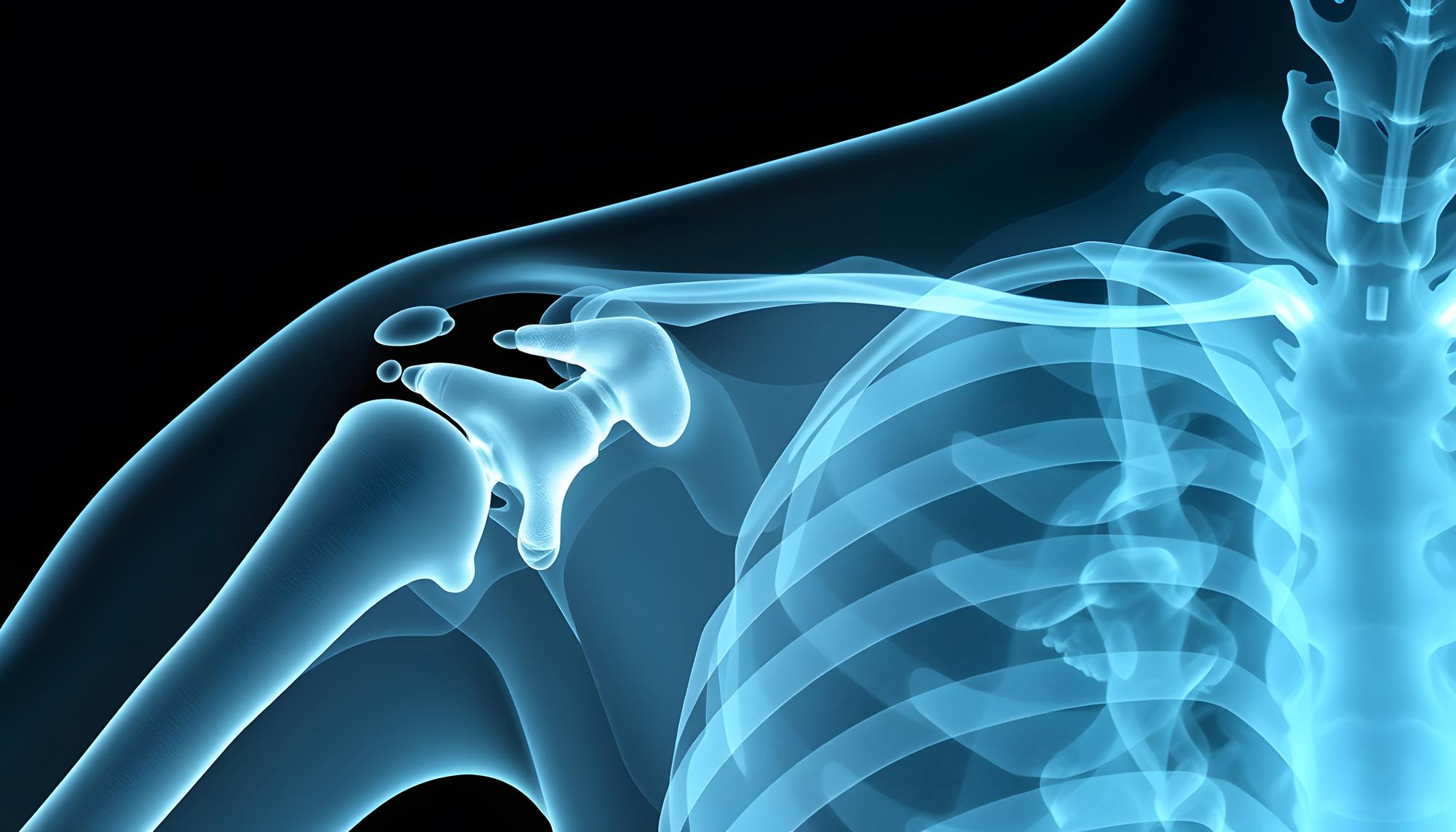
X-ray of a shoulder used for diagnosing frozen shoulder.
Treatment options for frozen shoulder
Here's what I tell every patient: the vast majority of frozen shoulders, around 90%, get better without surgery. But "getting better on its own" doesn't mean you should just wait it out. Treatment reduces pain, shortens the recovery timeline, and prevents permanent stiffness.
1. pain relief and anti-Inflammatory medications
During the freezing stage, when pain is severe, oral medications like NSAIDs (ibuprofen, naproxen) help control inflammation. I sometimes prescribe a short course of oral steroids for patients in acute pain. These aren't meant for long-term use — just to get the pain under enough control that the patient can start physiotherapy.
2. physiotherapy, The most important treatment
If I had to pick one treatment, it's this. Nothing else comes close to structured, guided physiotherapy for frozen shoulder. A trained physiotherapist will work on:
- Pendulum exercises (gentle arm swinging using gravity)
- Wall climbing stretches
- External rotation stretches using a stick or towel
- Cross-body stretches
- Progressive range-of-motion exercises as the shoulder loosens
The key is consistency. I tell patients: 15–20 minutes of stretching exercises at home, twice a day, every single day. Missing sessions slows recovery noticeably.
3. Hot and cold therapy
- Heat (warm towel or hot water bag) before exercises, it relaxes the muscles and makes stretching easier
- Ice packs after exercises — to reduce any inflammation triggered by the stretching
This simple routine makes a real difference in how comfortable the exercises feel.
4. corticosteroid injections
In the freezing stage, when pain is too severe for the patient to tolerate physiotherapy, a steroid injection directly into the shoulder joint can provide dramatic relief within 48–72 hours. It reduces inflammation inside the capsule and opens a window for physiotherapy to begin. Most patients need only 1–2 injections. I don't recommend more than 3, as repeated steroid injections can weaken the surrounding tissues.
5. hydrodilatation (Distension arthrography)
This is a procedure where sterile saline and a small amount of steroid are injected into the shoulder capsule under imaging guidance. The fluid stretches the capsule, physically breaking some of the adhesions. It's done as a daycare procedure, no admission needed, and can give immediate improvement in range of motion.
6. surgical options
Surgery is reserved for cases that haven't responded to 6–12 months of conservative treatment. The two main options are:
- Arthroscopic capsular release — tiny incisions, a camera goes inside, and the surgeon cuts through the thickened capsule. Recovery is quicker than open surgery.
- Manipulation under anaesthesia (MUA), the surgeon moves the shoulder through its full range while the patient is under general anaesthesia, breaking the adhesions. This is followed immediately by aggressive physiotherapy.
Both procedures have good outcomes, but physiotherapy after surgery is absolutely critical, without it, the capsule can tighten up again.
Home care for faster recovery
Here are practical things you can do at home to speed up healing:
- Do your prescribed stretching exercises twice daily — morning and evening work best
- Apply a warm compress to the shoulder for 10–15 minutes before stretching
- Avoid sudden or jerky arm movements, but don't keep the arm completely still either
- Sleep on the unaffected side with a pillow supporting the affected arm
- Wear front-open shirts or kurtas, pulling clothes over the head is painful and unnecessary
- Stay consistent with your physiotherapy appointments even when the pain improves (stiffness needs continued work)
- If you have diabetes, keep your blood sugar well controlled, high sugar levels slow healing

A woman stretching her shoulder to improve mobility.
Common misconceptions about frozen shoulder
"It will go away on its own — I just need to wait." Technically, yes, most frozen shoulders eventually resolve. But "eventually" can mean 2–3 years of pain and restricted function. Treatment shortens this dramatically and prevents permanent stiffness.
"I should rest my shoulder completely." This is one of the worst things you can do. Complete rest allows more adhesions to form. Gentle, guided movement within your pain tolerance is essential.
"Frozen shoulder means there's damage inside the joint." The joint surfaces and cartilage are perfectly fine. The problem is entirely in the capsule, the lining around the joint.
"It only happens to old people." I regularly see patients in their early 40s with frozen shoulder. Age 40–60 is the typical range.
When should you see a doctor?
Don't delay seeing a specialist if you notice:
- Shoulder pain lasting more than 2–3 weeks that isn't improving
- Difficulty raising your arm or reaching behind your back
- Night pain that disrupts your sleep
- Shoulder stiffness developing after a period of immobilization (fracture, surgery)
- You have diabetes or thyroid disease and notice new shoulder symptoms
Early intervention, even just starting the right exercises — can prevent a mild case from progressing to a severely frozen stage.
Early intervention, even just starting the right exercises, can prevent a mild case from becoming a severely frozen shoulder that takes a year or more to resolve.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.