Can physiotherapy prevent surgery? realistic expectations explained

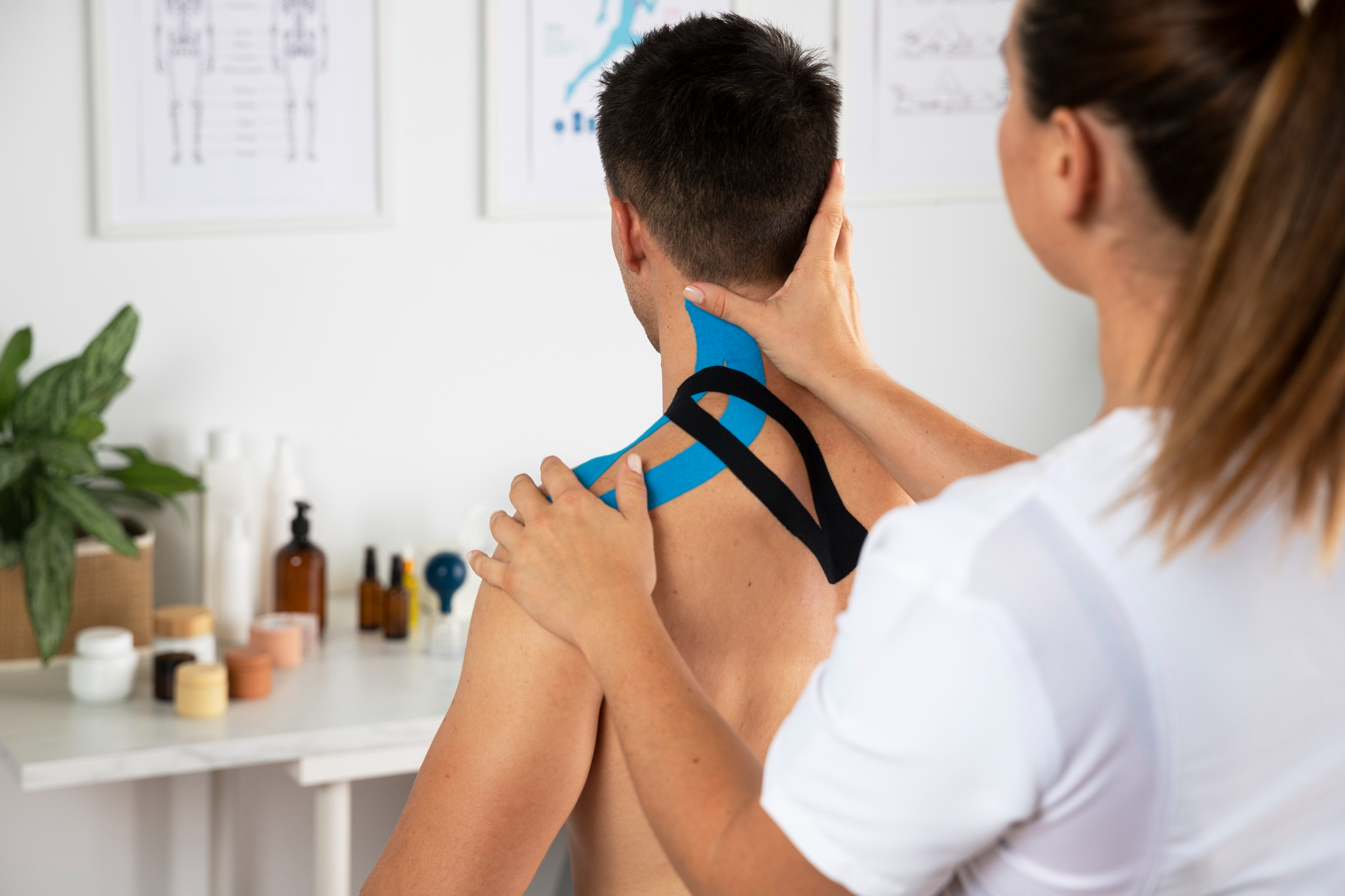
Physiotherapist guiding shoulder and arm movement during rehabilitation session
"Doctor, kya physiotherapy se kaam chal jayega ya surgery karni padegi?", I hear this question at least 3-4 times a day at my clinic. And it's a fair question. Surgery means hospital stays, anesthesia risks, rehab time, and costs that can run into lakhs. Nobody wants surgery if they can avoid it. But the flip side is equally dangerous: avoiding surgery when you genuinely need it, hoping physiotherapy will somehow fix a problem it was never designed to fix.
After 15+ years as an orthopedic surgeon at KDSG Hospital, Noida, I've seen both extremes. Patients who went through unnecessary surgeries because they weren't offered adequate physiotherapy first. And patients who delayed critical surgery for months, sometimes years — because they believed physiotherapy alone would cure a structural problem. Both groups suffered more than they needed to.
The truth sits somewhere in the middle. Physiotherapy can absolutely prevent surgery in specific conditions. In others, it can't, and pretending otherwise wastes time and risks permanent damage. Let me break down exactly when physiotherapy works, when it doesn't, and how to make the right call.
What physiotherapy actually does to your body
Physiotherapy isn't just "exercises." It's a structured clinical intervention that targets specific biomechanical problems. A trained physiotherapist works on:
- Restoring range of motion, After injury or prolonged immobility, joints stiffen. Graded mobilization techniques and stretching restore movement gradually.
- Strengthening weakened muscles — Muscles around an injured joint compensate for damaged structures. Strengthening them reduces load on the damaged area.
- Correcting movement patterns, Many injuries stem from how you move, not just what happened to you. Gait training, posture correction, and neuromuscular re-education address these root causes.
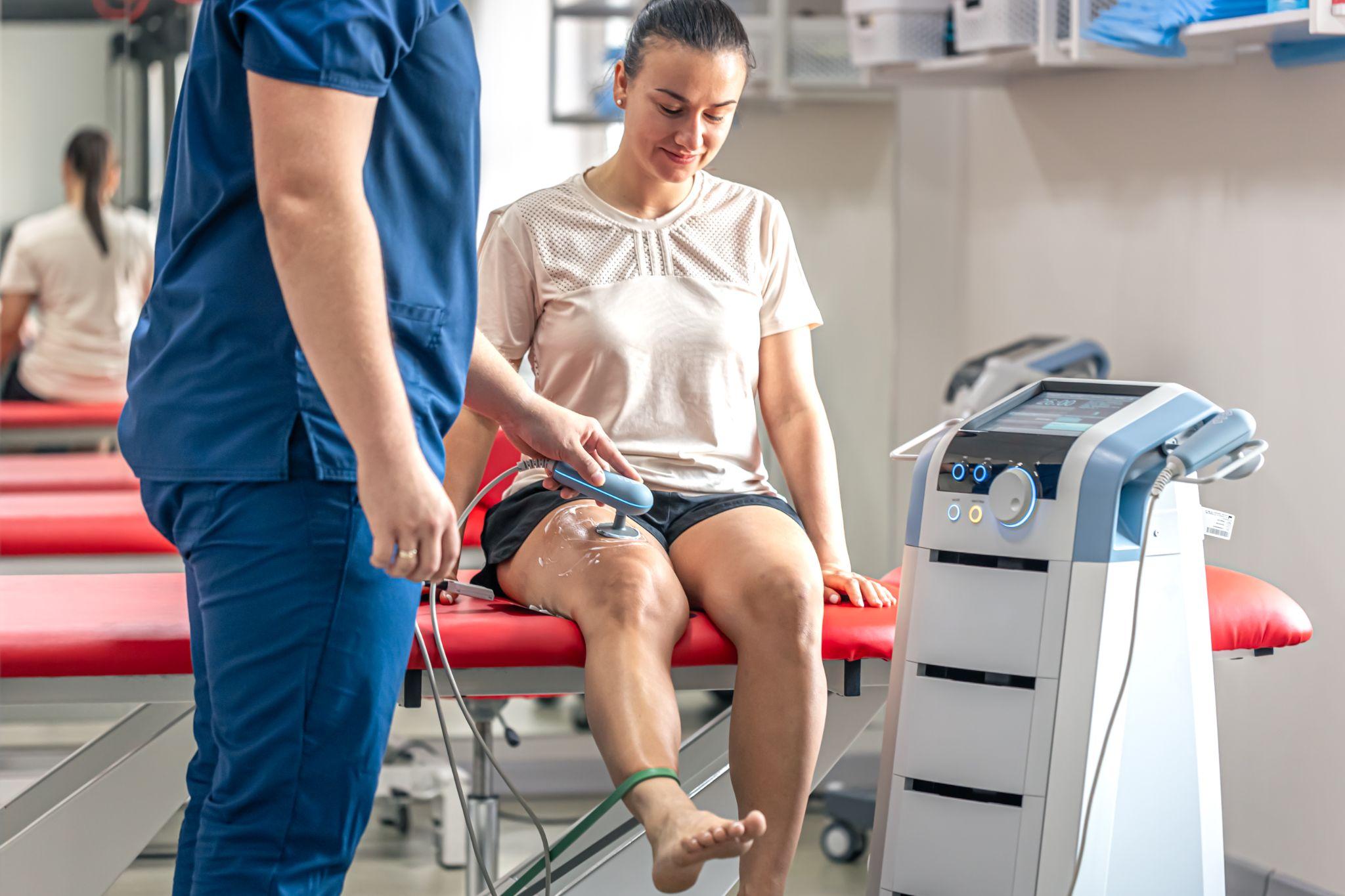
- Reducing pain and inflammation, Through modalities like ultrasound therapy, TENS (transcutaneous electrical nerve stimulation), ice/heat application, and manual therapy techniques.
- Preventing secondary complications — Muscle atrophy, joint contractures, and compensatory injuries that develop when the primary problem goes untreated.
Physiotherapy doesn't regenerate destroyed cartilage, reconnect completely torn ligaments, or realign deformed bones. Understanding this distinction is everything.
Conditions where physiotherapy Can genuinely help avoid surgery
Mild to moderate muscle strains and ligament sprains
Grade 1 and most Grade 2 ligament injuries, where the ligament is stretched or partially torn but still intact, respond well to physiotherapy. The protocol typically involves initial rest and ice (first 48-72 hours), followed by progressive strengthening of surrounding muscles. For a mild MCL (medial collateral ligament) sprain in the knee, for example, 4-6 weeks of structured physiotherapy achieves full recovery in about 85-90% of cases, with no surgery needed.
Timeline: 4-8 weeks for most mild-moderate sprains.
Early-Stage osteoarthritis (Grade 1-2)
When knee or shoulder arthritis is caught early — before significant cartilage loss, physiotherapy can reduce pain by 40-60% and delay surgical intervention by years. The mechanism is straightforward: stronger quadriceps and hamstrings absorb shock that would otherwise hammer the arthritic joint surface. Add weight management and activity modification, and many patients with early arthritis function well for 5-10 years without surgery.
I've had patients in their early 50s with Grade 2 knee osteoarthritis who, with disciplined physiotherapy and lifestyle changes, pushed their need for knee replacement into their mid-60s. That's a decade of avoiding major surgery.
Mechanical lower back pain
About 85-90% of lower back pain is "mechanical", caused by muscle weakness, poor posture, prolonged sitting, or disc dehydration. Not structural damage requiring surgical correction. Core strengthening, McKenzie exercises, and postural correction resolve most mechanical back pain within 6-12 weeks.
Red flags that suggest surgery might be needed instead: progressive leg weakness, loss of bladder or bowel control, or pain that doesn't improve at all after 6-8 weeks of dedicated physiotherapy.
Frozen shoulder (Adhesive capsulitis) — early and moderate stages
Frozen shoulder progresses through three stages: freezing (increasing pain, 2-9 months), frozen (stiffness peaks, 4-12 months), and thawing (gradual recovery, 5-24 months). In the freezing and early frozen stages, guided physiotherapy, specifically capsular stretching, pendulum exercises, and wall climbing exercises, can prevent the shoulder from reaching severe restriction.
Without intervention, some patients develop permanent restriction that requires manipulation under anesthesia or arthroscopic capsular release. Starting physiotherapy early, within the first 2-3 months of symptoms, significantly reduces this risk.
Post-Fracture rehabilitation
After a fracture heals (whether managed with a cast or with surgical fixation), the surrounding muscles atrophy, the joint stiffens, and movement patterns alter. Physiotherapy restores all three. Without it, patients often develop compensatory problems — a limp that causes hip pain, shoulder stiffness after a proximal humerus fracture, or knee contracture after a tibial plateau fracture.
In many cases, good post-fracture physiotherapy prevents the need for secondary corrective surgeries later.

Medical 3D rendering highlighting the shoulder joint structure with areas of pain and inflammation.

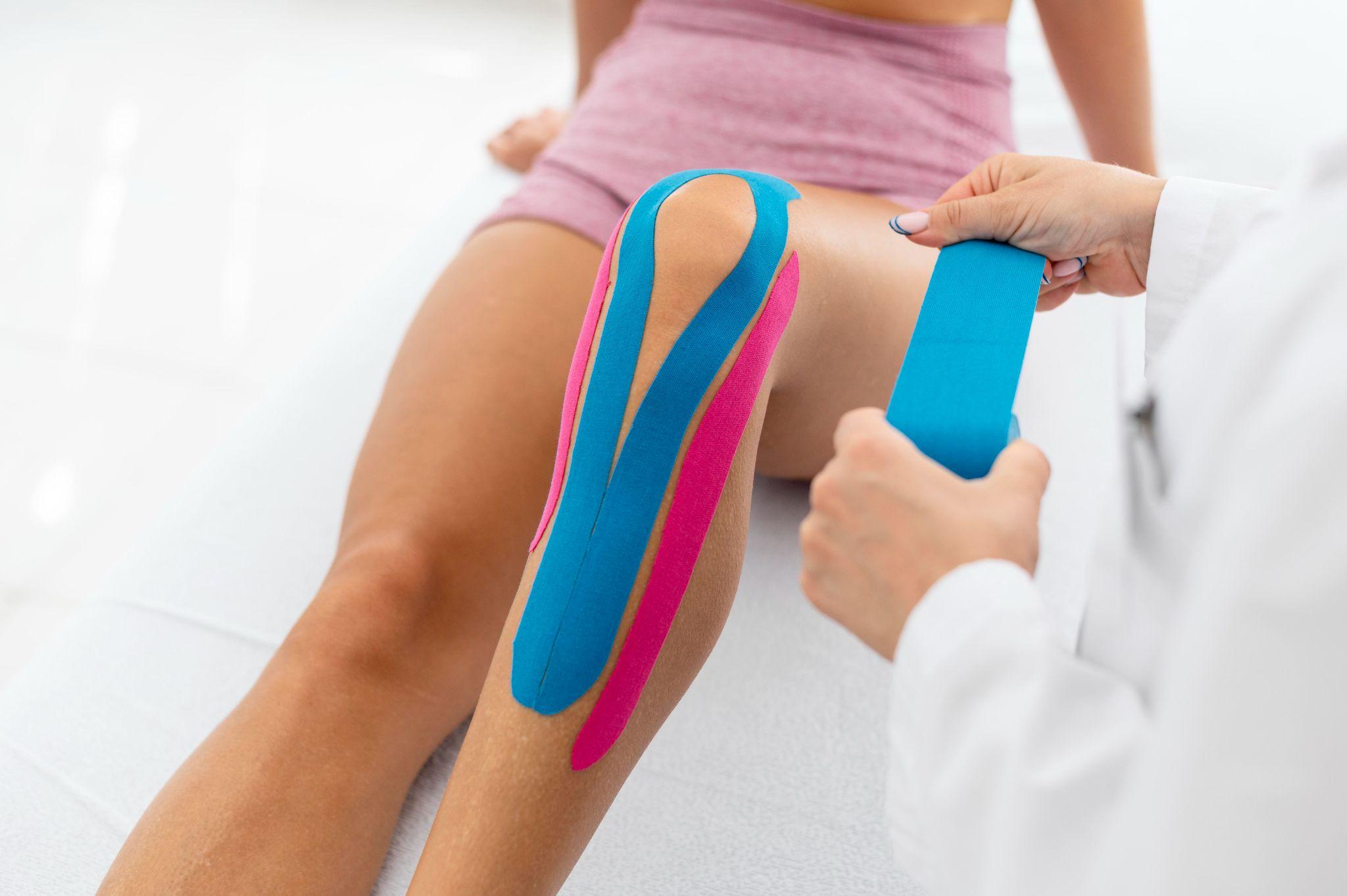
Physiotherapist using resistance band therapy for leg rehabilitation
Conditions where physiotherapy cannot replace surgery
This is where I see the most costly delays. Patients spend months in physiotherapy for problems that fundamentally require surgical repair.
Advanced osteoarthritis (Grade 3-4)
When cartilage is severely eroded, bone is grinding on bone, osteophytes (bone spurs) have formed, and the joint space has narrowed significantly on X-ray, no amount of muscle strengthening will restore that lost cartilage. Physiotherapy at this stage manages symptoms. It doesn't reverse the disease. If pain limits daily activities despite 3-6 months of physiotherapy, anti-inflammatory medications, and lifestyle modifications, joint replacement surgery becomes the most effective path forward.
Severe disc herniation with progressive neurological deficit
A bulging disc that causes occasional back pain and mild leg tingling? Physiotherapy works well for this. A large herniation compressing a nerve root, causing progressive foot drop, significant leg weakness (can't stand on toes or heels), numbness spreading to the groin, or loss of bladder/bowel control? That needs urgent surgical decompression — typically within 24-48 hours for cauda equina syndrome.
Every week of delay with a compressing nerve increases the risk of permanent nerve damage that no surgery can reverse.
Complete ligament or tendon tears
A completely torn ACL (anterior cruciate ligament) in an active person, someone who plays sports, runs, or has a physically demanding job, won't heal with physiotherapy. The torn ends retract and scar tissue can't replicate the ligament's function. ACL reconstruction surgery followed by 6-9 months of rehabilitation is the standard approach.
Similarly, a complete Achilles tendon rupture in an active individual, or a full-thickness rotator cuff tear causing significant weakness, typically requires surgical repair.
Grade 3 tears = surgery first, physiotherapy after. That's the general principle.
Structural deformities and malalignment
Severe bow legs (genu varum), knock knees (genu valgum), or angular deformities from malunited fractures need surgical correction — osteotomy, realignment procedures, or reconstructive surgery. Physiotherapy can't straighten bones.
However, pre-operative physiotherapy (prehabilitation) in these cases strengthens muscles and optimizes the body for surgery, leading to faster post-operative recovery.
Realistic recovery timelines with physiotherapy
One of the biggest frustrations I see is unrealistic expectations about speed. Physiotherapy is not a quick fix. Biological tissue takes time to adapt.
- Mild muscle strain: 2-4 weeks
- Moderate ligament sprain: 4-8 weeks
- Frozen shoulder: 3-9 months (sometimes up to 12-18 months for full resolution)
- Early arthritis management: Ongoing, with periodic reassessment
- Post-surgical rehabilitation (ACL, knee replacement): 6-12 months to full functional recovery
- Chronic lower back pain: 6-12 weeks for significant improvement, with ongoing maintenance exercises
Patients should expect gradual progress, not dramatic overnight improvement. If there's zero improvement after 4-6 weeks of consistent, supervised physiotherapy, it's time to reassess the diagnosis and consider whether the treatment plan needs to change.
How We decide between physiotherapy and surgery
The decision isn't arbitrary. As an orthopedic surgeon, I weigh specific clinical factors:
- Severity of structural damage, An MRI showing a partial ligament tear vs. a complete tear changes the treatment plan entirely.
- Functional impact, Can you walk? Climb stairs? Do your job? If the problem significantly limits daily function despite conservative treatment, surgery becomes more justified.
- Duration of symptoms — Acute injuries respond differently than chronic, longstanding problems.
- Response to conservative treatment, We typically trial 6-12 weeks of physiotherapy before considering surgery (unless there are urgent red flags).
- Patient age, activity level, and goals, A 25-year-old cricketer with an ACL tear has different needs than a 65-year-old with the same injury who walks for exercise.
Surgery is rarely the first recommendation. But when imaging, clinical examination, and failed conservative treatment all point toward it, delaying further doesn't help — it often makes the eventual surgery more complex.
Physiotherapy's role even when surgery Is needed
Even when surgery is the right answer, physiotherapy isn't irrelevant. It's essential, before and after.
Prehabilitation (pre-surgery physiotherapy): Strengthening muscles before surgery improves post-operative outcomes. A patient going into knee replacement with stronger quadriceps recovers faster, regains mobility sooner, and reports less pain. Studies show prehabilitation reduces hospital stay by 1-2 days on average.
Post-operative rehabilitation: After ACL reconstruction, rotator cuff repair, or joint replacement, structured physiotherapy determines the final outcome. The surgery fixes the structural problem; rehabilitation restores function. Skip it or do it halfheartedly, and you'll end up with a technically successful surgery but a functionally limited joint.
Physiotherapy and surgery aren't opposites. They're partners.
Common misconceptions worth correcting
"Pain always means I need surgery.", Most musculoskeletal pain doesn't require surgical intervention. Muscle spasms, tendinitis, bursitis, and postural strain cause significant pain but respond to conservative treatment.
"Physiotherapy can fix anything if I do it long enough." — No. Some problems are structural and need structural repair. Continuing physiotherapy for a condition it can't fix wastes time, money, and delays effective treatment.
"I should avoid all movement when something hurts.", Prolonged immobility actually worsens most orthopedic conditions. Guided, controlled movement promotes healing. Complete bed rest is rarely recommended beyond the first 24-48 hours for most injuries.
"If I need surgery, physiotherapy was a waste.", Pre-surgical physiotherapy isn't wasted time. It strengthens the body for surgery and often clarifies whether surgery is truly needed.
Making the right call
The decision between physiotherapy and surgery shouldn't be driven by fear of the operating room or blind faith in exercises. It should be driven by accurate diagnosis, objective imaging findings, clinical examination, and an honest discussion about what each treatment option can and can't achieve.
If you're unsure whether your condition requires surgery or can be managed with physiotherapy, get an assessment from an orthopedic specialist who'll give you a straight answer — not just the answer you want to hear. At KDSG Hospital, Noida, I work with patients to map out the most effective treatment path based on their specific diagnosis, activity level, and long-term goals. The aim isn't to avoid surgery at all costs, it's to find the treatment that gives you the best functional outcome with the least risk.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.