Back pain vs nerve pain: How to tell the difference

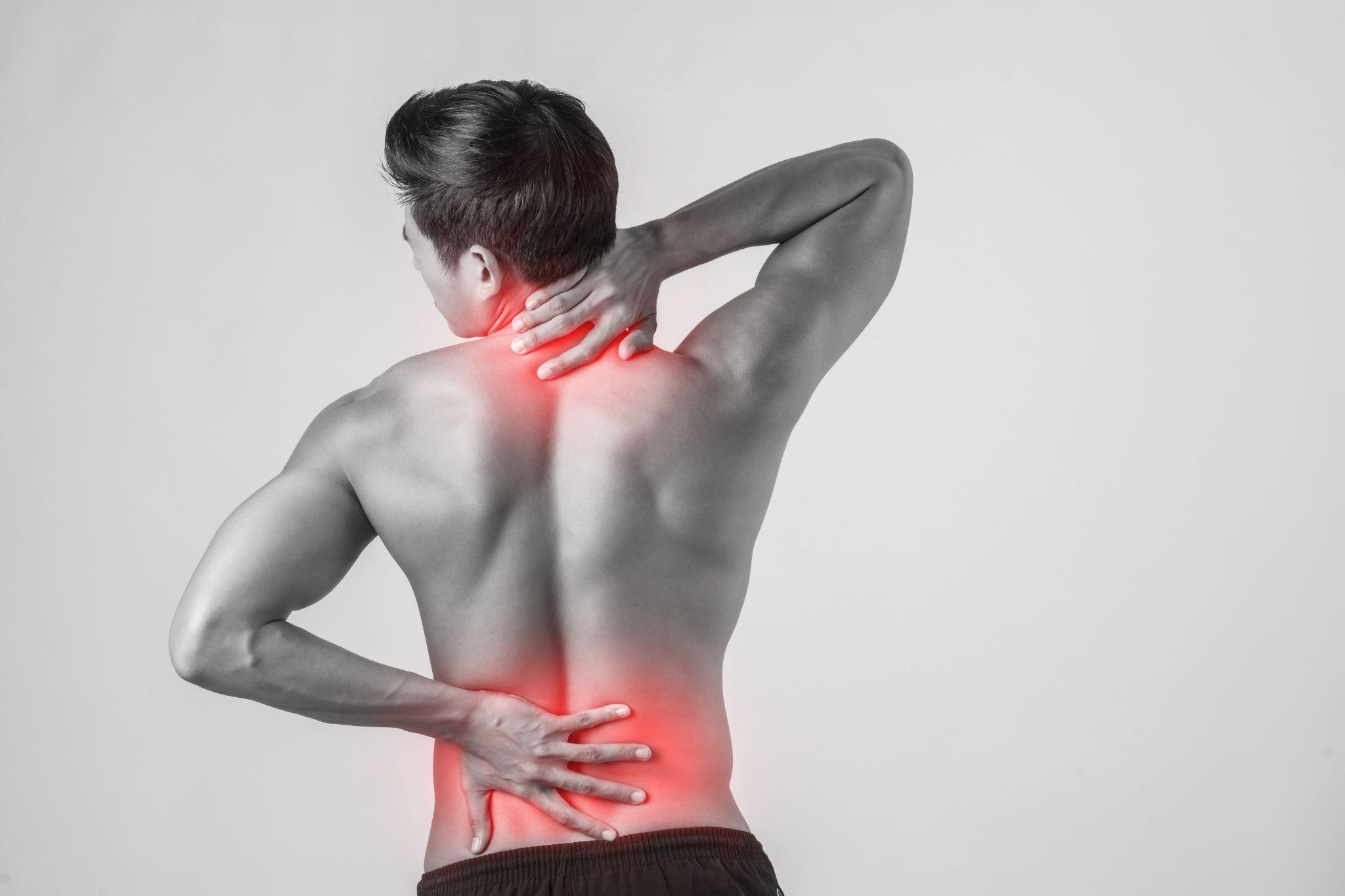
Woman experiencing upper and lower back pain indicating musculoskeletal strain
A patient walks into my clinic saying, "Doctor, my back hurts." That single complaint could mean fifty different things. It could be a strained muscle that'll settle in a week. Or it could be a compressed nerve that needs urgent attention. The difference between these two, back pain and nerve pain, changes everything about how we treat it, how long recovery takes, and what happens if it's ignored.
I'm Dr. Ankur Singh, senior orthopedic and spine surgeon at KDSG Superspeciality Hospitals, Noida. Over 15 years of practice, I've learned that the biggest obstacle to effective treatment isn't the condition itself. It's misidentification. Patients take the wrong painkillers for months. They do exercises that make things worse. They wait too long because they assume it's "just a muscle pull." By the time they reach a specialist, a problem that could've been resolved in two weeks has become a three-month ordeal.
This article breaks down how these two types of pain differ, what causes each, and when you absolutely need professional help.
What is back pain?
Back pain — also called musculoskeletal pain, originates from the muscles, ligaments, joints, or bones of the spine. It's structural. Something in the mechanical framework of your back is irritated, strained, or inflamed.
Common causes of back pain
- Muscle strain from overexertion, sudden awkward movements, or lifting something heavy with a rounded back
- Ligament sprain, overstretching the tough bands that hold your vertebrae together
- Degenerative disc disease — natural wear of the discs between vertebrae as you age
- Poor posture, slouching at a desk, hunching over a phone, sleeping on the wrong mattress
- Weak core muscles, when your abdominal and lower back muscles can't adequately support the spine, other structures compensate and get overloaded
- Facet joint irritation — the small joints at the back of each vertebra can become inflamed from arthritis or repetitive stress
Typical symptoms of back pain
- A dull, aching, or throbbing sensation
- Pain that stays localized, you can point to exactly where it hurts
- Stiffness, especially after waking up or sitting for a long time
- Pain that improves with gentle movement and stretching
- Worsening after prolonged sitting, standing, or physical exertion
- Tightness or spasm in the muscles along the spine
The hallmark of musculoskeletal back pain is its relationship with position and movement. It gets worse in certain postures, bending, lifting, sitting too long — and typically improves when you lie down or shift positions. Most episodes resolve within 2-6 weeks with appropriate care.
What is nerve pain?
Nerve pain, medically termed neuropathic pain, arises when a nerve is compressed, irritated, inflamed, or damaged. In the context of the spine, this usually happens when a spinal nerve root gets pinched by a herniated disc, a bone spur, or a narrowed spinal canal.
Common causes of nerve pain
- Herniated or bulging disc pressing on a nerve root — the single most common cause in patients under 50
- Spinal stenosis, narrowing of the spinal canal, more common after age 60
- Sciatica, compression of the sciatic nerve, typically from a lumbar disc herniation
- Cervical radiculopathy — a pinched nerve in the neck causing arm symptoms
- Spondylolisthesis, one vertebra slipping forward over another, trapping a nerve
- Bone spurs (osteophytes) from degenerative arthritis compressing nerves
- Diabetic neuropathy, nerve damage from poorly controlled blood sugar, though this follows a different pattern
Typical symptoms of nerve pain
- Sharp, shooting, or electric shock-like pain — patients often describe it as a "lightning bolt" or "current"
- Burning or searing sensation along the path of the nerve
- Tingling or pins-and-needles feeling, like your arm or leg "fell asleep" and won't wake up
- Numbness, actual loss of sensation in specific areas
- Pain that radiates — from the back down into the buttock, thigh, calf, or foot (sciatica), or from the neck into the shoulder, arm, and fingers
- Muscle weakness, difficulty lifting your foot, gripping objects, or climbing stairs
What distinguishes nerve pain from back pain is its traveling nature. It follows a specific nerve pathway. Sciatic nerve pain, for instance, traces a predictable route from the lower back through the hip, down the back of the thigh, and into the calf or foot. A patient can often draw the exact line of their pain on their body.

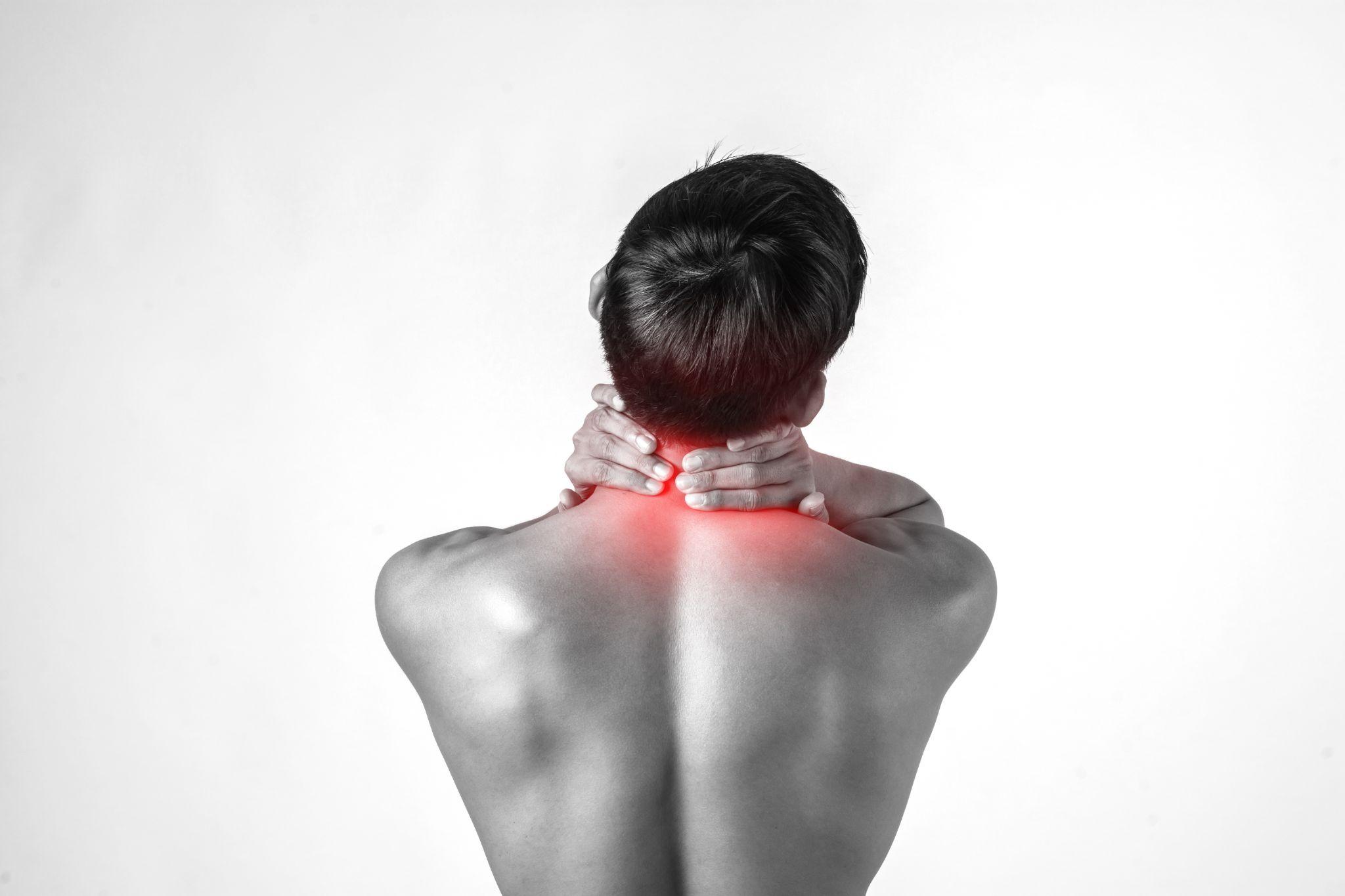
Illustration showing nerve-related pain radiating across the neck and upper back
Key differences between back pain and nerve pain
Nature of pain
Back pain feels dull, achy, sore, or tight. Like a muscle that's been overworked. Nerve pain is sharp, shooting, burning, more intense and more alarming. Patients with nerve pain frequently use words like "electric," "stabbing," or "searing." The quality of the pain alone often tells me which category we're dealing with.
Location
Back pain stays put. It affects the area around the spine — lower back, mid-back, or neck, and doesn't travel far from the source. Nerve pain radiates. It shoots down an arm or a leg, sometimes all the way to the fingers or toes. If your pain starts in the lower back and ends up in your calf, that's nerve involvement.
Triggers
Back pain worsens with mechanical stress, bending, lifting, prolonged sitting, physical labor. Change your position and it usually eases.
Nerve pain can be triggered by coughing, sneezing, or straining during a bowel movement — anything that momentarily increases pressure in the spinal canal. Sitting for a long period (especially driving) tends to aggravate sciatic nerve pain. Some patients report that even a slight shift in position sends a shooting pain down their leg.
Associated symptoms
Pure back pain doesn't cause numbness, tingling, or muscle weakness. If you're experiencing any of these alongside your back pain, a nerve is involved. Period. That's a clinical red flag that changes the urgency and the treatment approach.
Response to rest
Back pain generally improves with rest and position change. You lie down, the muscles relax, the pain fades.
Nerve pain doesn't follow that pattern. Many patients tell me their nerve pain is worse at night, it throbs, burns, or shoots when they're trying to sleep. Rest doesn't reliably help, and some positions (like lying flat) can actually increase nerve compression.
Can back pain turn into nerve pain?
Absolutely, and this is something I want every patient to understand. What starts as straightforward muscular back pain can progress to nerve pain if the underlying cause isn't addressed.
A common example: a patient has a mildly bulging disc causing localized lower back pain. They ignore it, continue heavy lifting, skip physiotherapy. Over months, the bulge worsens into a full herniation. The disc material pushes into the spinal canal and compresses a nerve root. Now they've got sciatica, radiating pain, tingling, weakness in the leg.
This progression isn't inevitable, but it's preventable. Early physiotherapy and lifestyle modification for back pain can stop it from becoming a nerve problem.

Conceptual illustration of spinal back pain focused on the lower spine
How doctors diagnose the difference
Accurate diagnosis requires a systematic approach. Here's what I do in my clinic:
Physical examination
- Observation — posture, gait, spinal alignment, any visible muscle spasm
- Palpation, feeling for tender spots, muscle tightness, trigger points
- Range of motion testing, which movements reproduce the pain
- Neurological assessment — testing reflexes, sensation (light touch, pinprick), and muscle strength in specific groups. A diminished ankle reflex, for instance, points to S1 nerve root compression.
- Provocative tests, Straight Leg Raise (SLR) test is highly reliable for lumbar nerve compression. If lifting a straight leg between 30-70 degrees reproduces shooting pain down the leg, it strongly suggests disc herniation.
Imaging and tests
- X-rays, show bone alignment, fractures, disc space narrowing, and arthritis. They don't show soft tissues like discs or nerves.
- MRI — the gold standard for diagnosing disc herniations, nerve compression, spinal stenosis, and soft tissue pathology. I order this when nerve involvement is suspected or when back pain doesn't respond to 4-6 weeks of treatment.
- CT scan, useful for detailed bone assessment, especially in older patients with stenosis
- Nerve conduction studies (NCS) and EMG, these measure electrical activity in nerves and muscles. Helpful when I need to confirm which nerve is affected and how severely it's damaged.
One important note: imaging findings don't always correlate with symptoms. Studies show that 30-40% of people with no back pain at all have disc bulges on MRI. This is why I always treat the patient, not the scan.
Treatment approaches differ
Treatment for back pain
Most musculoskeletal back pain responds well to conservative measures:
- Activity modification — avoid the specific triggers, but don't go to bed for days. Prolonged bed rest makes back pain worse, not better.
- Physiotherapy, core strengthening, flexibility work, postural correction. A good physiotherapy program is the single most effective treatment for recurrent back pain.
- Hot or cold therapy, ice for acute inflammation (first 48-72 hours), heat for muscle stiffness and spasm
- Over-the-counter pain relief — paracetamol or NSAIDs for short-term use
- Posture correction, ergonomic workstation setup, proper sleeping position (side-lying with a pillow between knees often helps), avoiding prolonged static positions
- Regular walking, 30 minutes of daily walking is one of the best things you can do for a sore back
Most patients with acute back pain recover within 4-6 weeks. For chronic back pain (lasting over 3 months), a structured rehab program is essential.
Treatment for nerve pain
Nerve pain requires a different strategy:
- Nerve-specific medications — standard painkillers often don't work well for nerve pain. Drugs like pregabalin, gabapentin, or duloxetine target nerve signaling and are far more effective.
- Physiotherapy focused on nerve mobilization, specific exercises that gently glide the affected nerve through its pathway, reducing adhesions and irritation. Neural flossing exercises are particularly useful for sciatica.
- Epidural steroid injections, for moderate to severe radiculopathy, a targeted injection of corticosteroid around the compressed nerve root can significantly reduce inflammation and pain. I recommend this when medications and physio alone aren't providing enough relief.
- Nerve root blocks — diagnostic and therapeutic injections that pinpoint the exact nerve causing symptoms
- Surgery, indicated when there's progressive weakness, loss of bladder or bowel control, or pain that doesn't respond to 6-8 weeks of aggressive non-surgical treatment. Microdiscectomy for disc herniations and decompression surgery for stenosis have high success rates.
The critical point: regular painkillers like paracetamol or ibuprofen barely touch nerve pain. If you've been taking these for weeks without relief and your pain shoots down your arm or leg, you're likely dealing with a nerve issue that needs different medication and a proper evaluation.
When should You See a doctor?
Seek medical attention, don't wait — if you experience:
- Pain that persists beyond two weeks without improvement
- Radiating pain into your arms, hands, legs, or feet
- Numbness, tingling, or pins-and-needles sensation
- Weakness in your limbs, dropping things, foot dragging, difficulty climbing stairs
- Loss of bladder or bowel control, this is a surgical emergency (cauda equina syndrome)
- Pain that's worse at night or wakes you from sleep
- Back pain accompanied by unexplained weight loss or fever
These aren't symptoms to manage with home remedies or YouTube exercises. They require clinical assessment to rule out serious spinal pathology.
Why early diagnosis matters
Ignoring nerve pain is risky. Prolonged nerve compression can cause permanent damage — chronic numbness, lasting weakness, muscle wasting. I've treated patients who waited a year with worsening sciatica, and by the time they came in, the nerve damage was partially irreversible. They recovered, but not completely. Earlier intervention would have made a full recovery achievable.
For musculoskeletal back pain, early physiotherapy and postural correction prevent the common cycle of repeated episodes. Most people who have one episode of back pain will have another, unless they address the underlying weakness or imbalance that caused it.
Final word
Back pain and nerve pain may overlap, but they're fundamentally different problems. Back pain is mechanical, muscles, ligaments, joints. It stays localized, responds to rest and posture changes, and rarely causes numbness or weakness. Nerve pain is electrical — sharp, shooting, burning. It travels along a specific nerve path, causes tingling or numbness, and doesn't respond to ordinary painkillers.
The nature of your pain, where it goes, and what symptoms accompany it, these clues are diagnostic gold. Pay attention to them. Describe them clearly to your doctor.
If you're dealing with persistent back or radiating pain, accurate diagnosis is the first step toward effective treatment. At KDSG Superspeciality Hospitals in Noida, I use a thorough clinical and imaging-based approach to determine exactly what's causing your pain and build a treatment plan that addresses the root cause, not just the symptoms.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.