Football injuries: An orthopaedic guide to common injuries, treatment, and prevention

Football player holding knee after injury on field.
Why football carries such a high injury risk
Football places extraordinary demands on the human body. A single match can involve 10–13 kilometres of running, hundreds of directional changes, aerial duels, slide tackles, and bursts of sprinting at near-maximum effort. Each of these actions loads joints, muscles, tendons, and ligaments in ways that push them close to their structural limits.
I've treated professional players as well as weekend warriors who play five-a-side on synthetic turf after work. The injury patterns are remarkably similar, what changes is the mechanism. A professional might tear an ACL during a competitive tackle; a recreational player tears the same ligament stepping into a divot on an uneven field. Conditioning differences, footwear choices, and playing surface all feed into the risk equation.
Two factors make football uniquely dangerous compared to, say, running or swimming. First, contact is inherent to the sport. You can't legislate away 50-50 challenges entirely. Second, the multidirectional nature of play, cutting, pivoting, decelerating — creates shearing forces across the knee, ankle, and hip that straight-line sports simply don't produce.
The most common football injuries I See in clinic
ACL, MCL, and PCL tears (Knee ligament injuries)
The knee absorbs the brunt of football's punishment. Ligament injuries here range from mild sprains to full-thickness ruptures.
- ACL (anterior cruciate ligament) tears typically happen without contact, the player plants a foot to change direction, and the knee gives way. There's an immediate "pop," followed by rapid swelling within two to four hours. An ACL rupture almost always requires surgical reconstruction if the player intends to return to pivoting sports.
- MCL (medial collateral ligament) injuries result from a direct blow to the outside of the knee, forcing it inward. Grade I and II MCL sprains usually heal with bracing and physiotherapy over four to six weeks. Grade III tears may need surgical repair.
- PCL (posterior cruciate ligament) injuries are less common and generally occur when a player falls on a bent knee or receives a hard tackle from the front. Many PCL injuries can be managed non-surgically, but combined ligament injuries often demand operative intervention.
In my practice, ACL tears account for the single largest category of football-related surgeries. The average recovery timeline after ACL reconstruction is nine to twelve months, a timeline that's non-negotiable if you want a durable outcome.
Meniscus tears
The meniscus is a C-shaped cartilage cushion between the femur and tibia. It distributes load, absorbs shock, and stabilises the knee. Rapid twisting or a deep squat under load can tear it.
Symptoms include:
- Sharp pain along the joint line
- Swelling that develops over 24–48 hours
- A clicking or catching sensation during movement
- Occasional "locking" — the knee gets stuck in a bent position
Small tears in the vascular (red) zone of the meniscus can sometimes heal with rest. Larger or displaced tears, especially bucket-handle tears that cause locking, usually require arthroscopic surgery, either repair with sutures or partial removal. Leaving a significant meniscus tear untreated accelerates cartilage wear and raises the risk of early-onset osteoarthritis.
Ankle sprains and chronic instability
Ankle sprains are arguably the most frequent acute injury on the football pitch. The typical mechanism is an inversion injury, the foot rolls inward, stretching or tearing the lateral ligaments (most commonly the anterior talofibular ligament).
A first-time mild sprain heals in two to three weeks with RICE (rest, ice, compression, elevation) and graduated rehabilitation. But here's the catch: studies show that up to 40% of people who sprain an ankle once go on to develop chronic ankle instability if rehabilitation is incomplete. Chronic instability means repeated giving way, persistent swelling, and difficulty playing on uneven surfaces. Some of these patients eventually need ligament reconstruction surgery — the Brostrom procedure, to restore stability.
Muscle strains and tears
Hamstring strains top the list, followed by quadriceps and calf injuries. These occur during explosive acceleration, deceleration, or over-stretching (think a lunging tackle). Grading runs from Grade I (mild fibre disruption, one to two weeks recovery) to Grade III (complete rupture, possible surgical repair and months of rehabilitation).
Fatigue is the single biggest risk factor. Muscles that are tired lose their eccentric braking capacity, and that's precisely when a hamstring tear happens, during the late swing phase of sprinting, when the hamstring must decelerate the lower leg.
Stress fractures
These overuse injuries develop when repetitive loading outpaces the bone's ability to remodel. The metatarsals (foot bones) and tibia (shin) are the most common sites in footballers. The pain typically starts as a dull ache that worsens with activity and improves with rest.
If a player pushes through a stress fracture, the incomplete fracture can propagate into a complete break. Treatment is straightforward but demands patience: six to eight weeks of protected weight-bearing, correction of training errors, and sometimes a bone stimulator for recalcitrant cases.
Warning signs that demand orthopaedic evaluation
Not every ache after a match warrants an MRI. But certain patterns shouldn't be brushed off:
- Joint pain that persists beyond 48–72 hours after play
- Swelling that recurs with every training session
- Any sensation of the knee "giving way" or shifting
- Restricted range of motion that doesn't improve with gentle stretching
- Pain that worsens progressively over weeks, rather than improving
Ignoring these signals doesn't make you tough — it converts a treatable problem into a chronic one.
How We diagnose football injuries
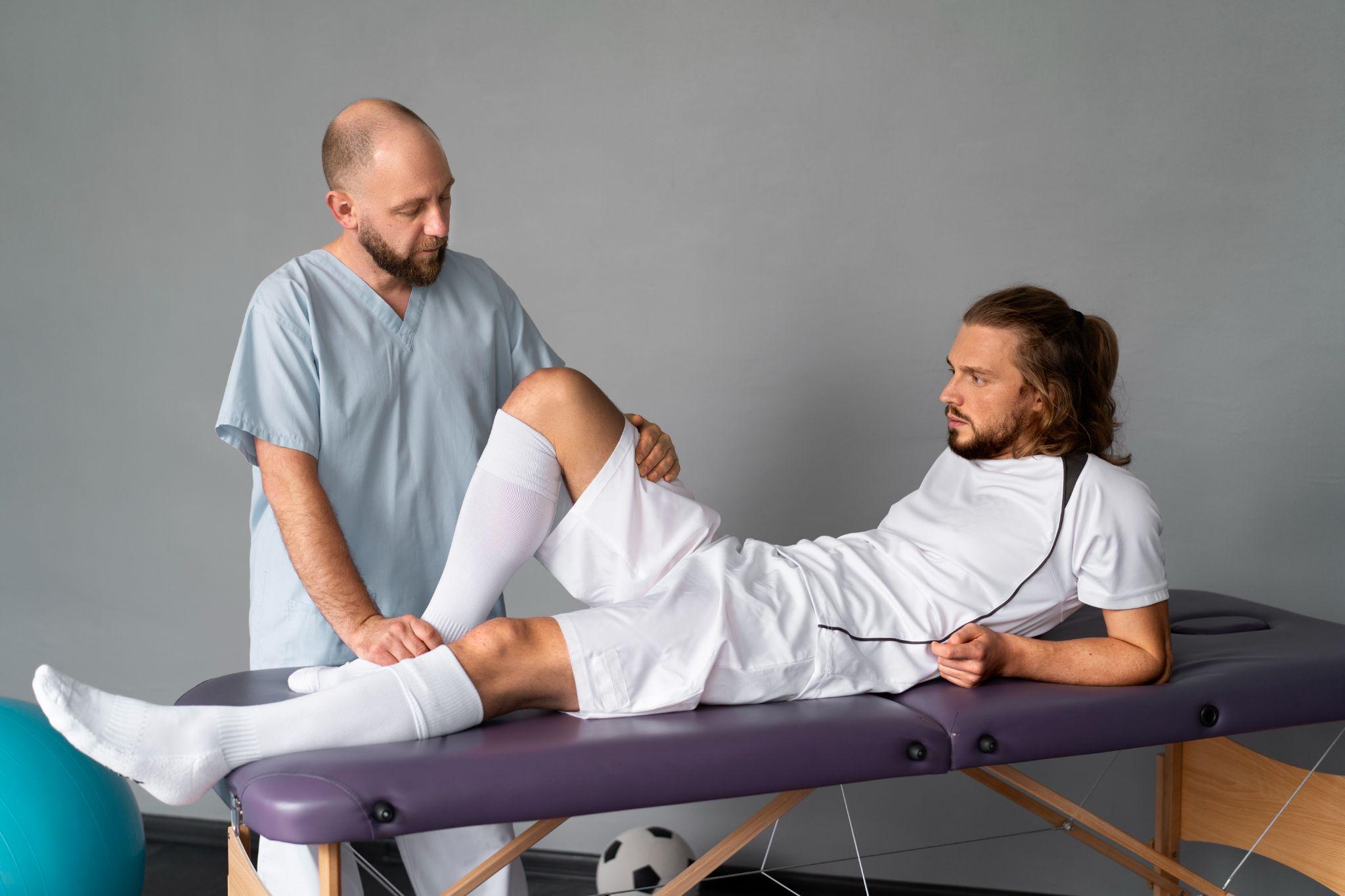
Orthopaedic doctor examining football player's knee during treatment.
A thorough clinical examination is still the foundation. Specific provocative tests, the Lachman test for ACL integrity, the McMurray test for meniscus tears, the anterior drawer test for ankle ligaments, give us a strong working diagnosis before any imaging.
X-rays are ordered first to rule out fractures and assess bony alignment. They're fast, inexpensive, and widely available.
MRI (magnetic resonance imaging) is the gold standard for soft tissue evaluation. It shows ligament tears, meniscal damage, cartilage defects, bone bruising, and muscle injuries with excellent resolution. I order an MRI when the clinical picture suggests a significant structural injury or when symptoms don't resolve as expected.
Ultrasound has a growing role for muscle and tendon injuries — it's dynamic, meaning we can visualise structures while the patient moves, and it provides real-time guidance for injections.
Getting the diagnosis right early saves time, money, and, most critically, prevents inappropriate activity that could worsen the injury.
Treatment approaches
Non-Surgical management
Many football injuries respond well to conservative care:
- Relative rest and activity modification — not necessarily complete immobilisation, but avoiding the specific movements that aggravate the injury.
- Structured physiotherapy, a progressive programme that restores range of motion, rebuilds strength, and retrains neuromuscular control. This isn't generic gym work; it's sport-specific rehabilitation.
- Cryotherapy and anti-inflammatory medication, useful in the acute phase to control swelling and pain. NSAIDs like ibuprofen are effective short-term but shouldn't be relied on for weeks.
- PRP (platelet-rich plasma) injections — increasingly used for tendon injuries and partial muscle tears. The evidence is evolving, but results in clinical practice have been encouraging for specific indications.
Surgical treatment
Surgery becomes necessary when the injury involves complete structural disruption, a full ACL tear in a player who wants to return to pivoting sports, a locked bucket-handle meniscus tear, a displaced fracture, or recurrent ankle instability that hasn't responded to rehabilitation.
Modern arthroscopic techniques allow most knee and ankle procedures to be performed through small incisions (typically 5–10 mm). This means less tissue damage, reduced post-operative pain, and faster initial recovery compared to open surgery. ACL reconstruction uses tendon grafts (hamstring or patellar tendon) to replace the torn ligament, and fixation techniques have improved significantly over the past decade.
Rehabilitation and return to play

Football player dribbling ball on grass field during match after recovery.
Rehabilitation isn't an afterthought, it's the treatment. A well-performed surgery with poor rehab produces a worse outcome than a simpler injury with excellent rehab.
Return-to-play criteria that I use in my practice include:
- Pain-free full range of motion — the injured joint must move as freely as the uninjured side.
- Strength symmetry, quadriceps and hamstring strength within 90% of the opposite leg, measured on an isokinetic dynamometer.
- Functional testing, hop tests, agility drills, and sport-specific movements performed at match intensity without apprehension.
- Psychological readiness — fear of re-injury is real and can alter movement patterns, increasing the risk of a second injury.
Cutting corners on rehabilitation is the single most common reason players get re-injured. I've seen too many patients rush back at six months after ACL surgery, only to tear the graft or injure the opposite knee.
Preventing football injuries before they happen
Dynamic warm-Up protocols
Static stretching before a match is outdated. Dynamic warm-ups, high knees, lunges, lateral shuffles, controlled sprinting, prepare muscles and joints for the demands ahead. The FIFA 11+ programme, specifically designed for football, has been shown to reduce injuries by 30–50% in teams that use it consistently.
Strength and balance training
Strong quadriceps, hamstrings, and gluteal muscles protect the knee. Core stability protects the lower back and pelvis. Single-leg balance exercises on unstable surfaces train proprioception — the body's ability to sense joint position, which is critical for avoiding awkward landings.
Footwear and playing surface
Studs that are too long for a hard surface increase rotational forces on the knee. Worn-out boots with degraded cushioning raise the risk of stress fractures. Artificial turf behaves differently from natural grass; players should adjust their footwear accordingly.
Periodisation and rest
Overuse injuries thrive on monotony and insufficient recovery. Training should cycle through phases of high and low intensity. Rest days aren't optional, they're when the body repairs microdamage and builds resilience.
The long-Term cost of untreated football injuries
A meniscus tear left alone for years leads to cartilage loss and eventually osteoarthritis — sometimes by a player's mid-thirties. Chronic ankle instability causes osteochondral lesions (damage to the cartilage lining the joint). Repeated hamstring strains create scar tissue that limits flexibility and predisposes to further tears.
Early orthopaedic treatment doesn't just fix the immediate problem. It preserves joint health for decades to come.
When to seek help
If you're dealing with a football injury that isn't settling, or if you want a pre-season screening to identify vulnerabilities before they become problems, sports injuries are a core part of my practice. I tailor treatment plans to each player's goals, whether that's returning to a competitive league or simply enjoying a weekend kickabout without pain.
Schedule an appointment with Dr. Ankur Singh at KDSG Hospital, Noida for personalised orthopaedic care built around your sport and your body.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.