Are flat feet causing You more problems than You think?
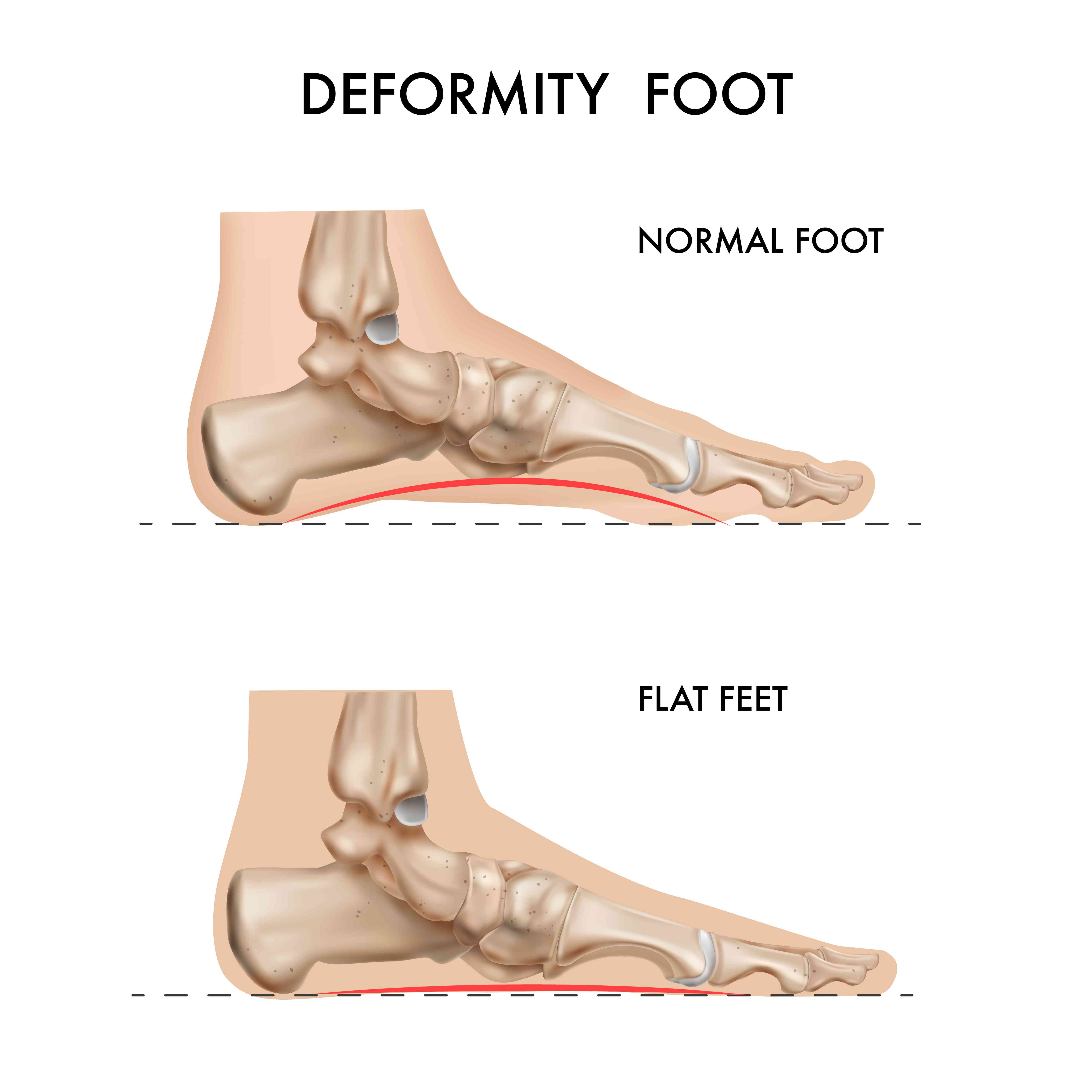
Comparison between a normal foot and a flat foot, highlighting the absence of a natural arch in flat feet.
A patient walked into my clinic last month with chronic knee pain. She'd been to multiple doctors, tried painkillers, even got knee X-rays, everything looked normal. When I asked her to take off her shoes and stand, the problem was obvious. Both feet were completely flat. No arch at all. Her knees had been absorbing shock that the foot arch should have been handling for years.
This is more common than people realize. Flat feet, medically called pes planus — affect roughly 20-30% of the Indian population. Most people don't even know they have them until the damage shows up somewhere else entirely: the knees, the hips, the lower back.
What exactly Are flat feet?
Your foot has a natural arch on the inner side, it's the curved gap between the ball of your foot and the heel when you stand. This arch acts as a spring-loaded shock absorber. Every time your foot hits the ground, the arch compresses slightly and then rebounds, distributing the impact evenly.
In flat feet, this arch is either absent or has collapsed. The entire sole makes contact with the ground. Some people are born this way, the arch simply never developed during childhood (it usually forms between ages 3-6). Others develop flat feet later in life when the posterior tibial tendon, which supports the arch, weakens or tears.
There are two types that matter clinically:
- Flexible flat feet: The arch disappears when standing but reappears when you sit or stand on your toes. This is the more common and generally milder type.
- Rigid flat feet: The arch is absent regardless of position. This type is more likely to cause pain and functional problems.
Symptoms that point to flat feet problems
Not everyone with flat feet has symptoms. I see plenty of patients with completely flat arches who run, play sports, and live pain-free. The arch itself isn't the issue — the problem starts when the flat foot changes how forces travel through your body.
Watch for these signs:
- Foot pain, particularly along the inner ankle, the arch area, or the heel. Worse after standing or walking for extended periods
- Ankle rolling inward, you might notice your shoes wear unevenly, with the inner sole wearing out faster
- Shin pain — especially during or after running. Flat feet are a leading cause of shin splints in young athletes
- Knee pain, the inward rolling of the ankle (overpronation) rotates the shin bone, putting abnormal stress on the knee joint
- Lower back ache, when the feet don't absorb shock properly, the spine picks up the slack
- Tight Achilles tendon — the calf muscles and Achilles often shorten to compensate for the flat arch
- Difficulty standing on tiptoe, this can indicate posterior tibial tendon dysfunction
How flat feet affect your entire body
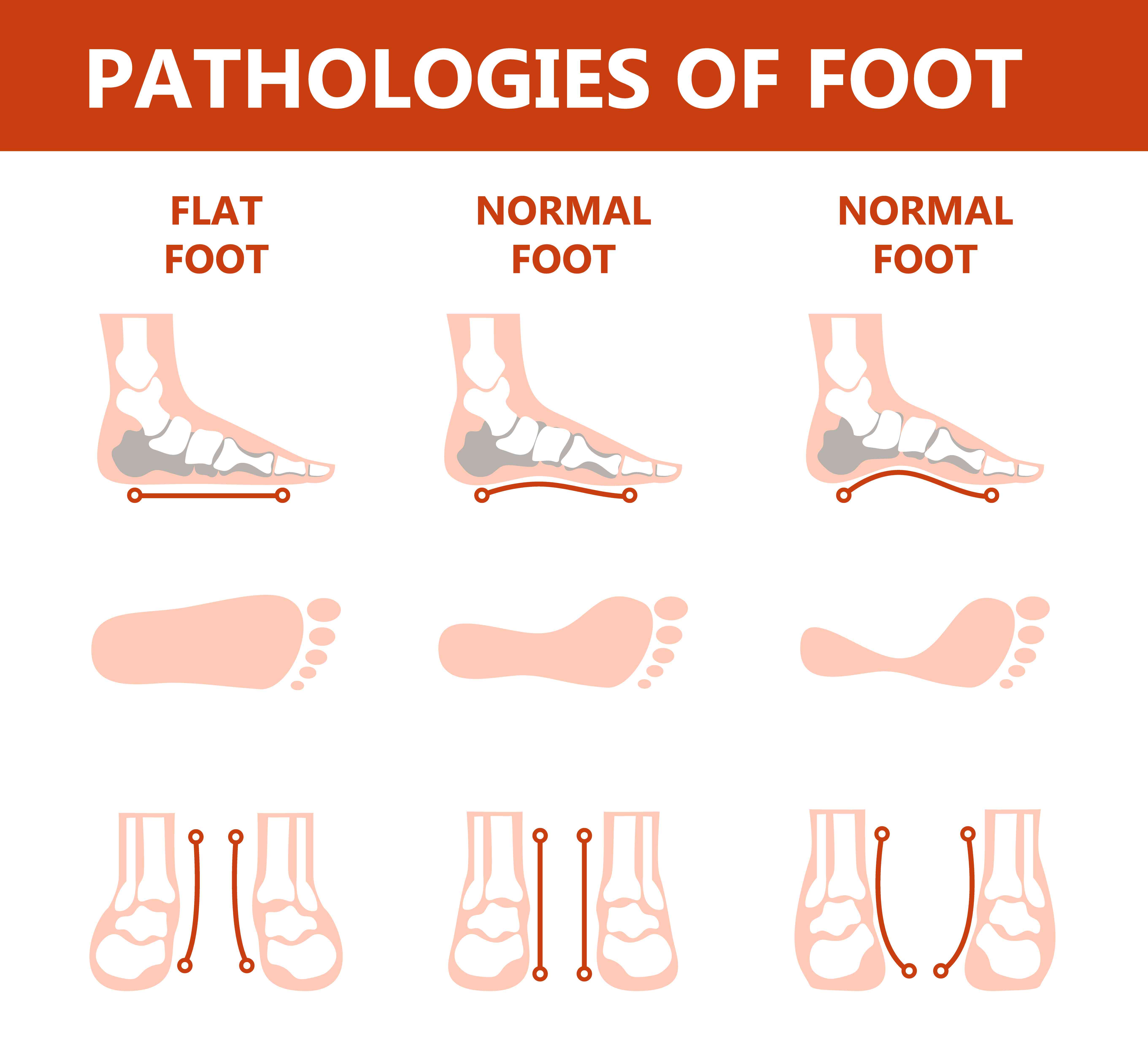
Visual representation of foot pathologies, illustrating the structural and imprint differences of flat feet versus normal feet.
This is the part most people miss. Your foot is the foundation of your entire skeletal structure. When the foundation tilts, everything above it compensates.
The chain reaction looks like this:
Flat foot → ankle rolls inward (overpronation) → shin bone rotates internally → knee falls inward (valgus stress) → hip drops on one side → pelvis tilts → lower back curves abnormally → neck and shoulder tension
I've treated patients whose chronic neck pain traced all the way back to their feet. It sounds dramatic, but biomechanics doesn't lie. When I correct their foot alignment with proper orthotics, the neck pain often improves within weeks, without ever touching the neck.
Conditions directly linked to flat feet
If you have flat feet and develop any of these conditions, there's likely a connection:
- Plantar fasciitis — the most common complication. The plantar fascia (a thick band running along the sole) gets overstretched when there's no arch support. This causes stabbing heel pain, especially with the first steps in the morning.
- Achilles tendinitis, the Achilles tendon works overtime to stabilize a flat foot, leading to inflammation and pain at the back of the ankle.
- Shin splints, common in runners and military recruits with flat feet. The tibialis posterior muscle overworks trying to maintain the arch.
- Bunions — flat feet change the angle of force through the big toe joint, gradually pushing it outward.
- Knee osteoarthritis, studies show that people with flat feet have a higher incidence of medial (inner) knee arthritis because of the altered load distribution. I see this regularly in patients over 50.
- Posterior tibial tendon dysfunction (PTTD), the tendon that holds up the arch can progressively weaken, causing the arch to collapse further over time. This is the most serious complication and may eventually need surgery.
Diagnosing flat feet
Many people walk around with flat feet for decades without knowing. Diagnosis is straightforward:
Wet footprint test (you can do this at home): Wet your feet, stand on a flat surface like a dark tile or paper bag. If your footprint shows the entire sole without a gap on the inner side, you have flat feet.
Clinical examination: I'll watch you walk (gait analysis), check whether your arch appears when you stand on tiptoes (flexible vs. rigid), test the strength of your posterior tibial tendon, and look at how your shoes have worn down.
Imaging when needed:
- X-rays (weight-bearing): Show the bone alignment and measure specific angles that confirm the degree of flatness
- MRI: If I suspect a tendon tear, particularly the posterior tibial tendon
- CT scan: Rarely needed, but useful for complex bony deformities or before surgical planning
Treatment: what actually helps

Custom orthopedic insoles provide essential support and relief for individuals with flat feet.
Treatment depends on whether your flat feet are causing symptoms and how severe they are.
Arch support and orthotics
For most symptomatic flat feet, custom or semi-custom orthotic insoles are the first line of treatment. These inserts fit inside your regular shoes and recreate the arch support your foot lacks.
Over-the-counter insoles from a good pharmacy can work for mild cases. For moderate to severe flat feet, I recommend custom-molded orthotics made from a plaster cast of your foot. They cost more (typically Rs 3,000-8,000) but last 2-3 years and provide far better support.
Footwear changes
This is free and makes a real difference. Avoid completely flat shoes — no flip-flops, no flat sandals, no ballerina flats for extended walking. Look for shoes with built-in arch support and a firm heel counter (the back part that cups your heel). Motion-control running shoes are specifically designed for overpronators.
Exercises that strengthen the arch
Towel scrunches: Place a towel on the floor. Using only your toes, scrunch it toward you. 3 sets of 15 reps, daily.
Heel raises: Stand on the edge of a step, lower your heels below the step level, then rise up onto your toes. Slow and controlled. 3 sets of 12.
Short foot exercise: While sitting, try to shorten your foot by pulling the ball of your foot toward the heel without curling the toes. This activates the intrinsic foot muscles that support the arch. Hold 10 seconds, repeat 15 times.
Calf stretches: Stand facing a wall, one foot forward, one back. Keep the back heel on the ground and lean into the wall until you feel a stretch in the calf. Hold 30 seconds each side, twice daily. Tight calves worsen flat foot mechanics.
Physical therapy
For flat feet causing significant pain or functional limitation, a structured physiotherapy program targeting ankle stability, calf flexibility, and foot muscle strength can produce meaningful improvement over 8-12 weeks.
Surgery (When conservative treatment fails)
Surgery is considered when:
- Pain persists despite 6+ months of orthotics, exercises, and physiotherapy
- The posterior tibial tendon is significantly torn or non-functional
- The deformity is rigid and progressive
- Arthritis has developed in the foot joints
Surgical options include tendon reconstruction, osteotomy (cutting and realigning bones), and in severe cases, joint fusion. Recovery takes 3-6 months but results are generally good.
Flat feet in children: when to worry
All babies and toddlers have flat feet, this is completely normal. The arch typically develops by age 5-6. In some children, it takes until age 8-10.
Bring your child to an orthopedic specialist if:
- They complain of foot or leg pain during or after activity
- They tire quickly and avoid physical activity
- Their shoes wear out unusually fast or unevenly
- The flat foot is stiff (rigid) rather than flexible
- Only one foot is affected (asymmetric flat foot needs evaluation)
Most childhood flat feet require no treatment, just monitoring. Rigid flat feet or those causing pain may benefit from custom orthotics or, rarely, surgery.
When to See a doctor
Don't ignore flat feet if you're experiencing:
- Persistent foot, ankle, or knee pain that hasn't responded to rest
- Difficulty walking or standing for normal durations
- One foot becoming progressively flatter than the other
- Swelling along the inner ankle
- Inability to stand on your tiptoes on the affected side
A flat foot itself isn't a disease. But a flat foot that's causing pain, limiting your activity, or creating problems elsewhere in your body deserves proper evaluation. The earlier we address it, the more options we have — and the less damage accumulates in the knees, hips, and spine over time.
Medical Disclaimer
The information provided on this website is for educational purposes only and should not be considered as medical advice. Please consult Dr. Ankur Singh or a qualified healthcare professional for personalized medical guidance.